Hemothorax is a bleeding into the pleural cavity. Mostly hemothorax occurs due to damage of the organs and walls of the chest, and can occur both in open and closed injuries.
The causes and mechanisms of development
Depending on the causes of hemothorax are:
- dramaticheskith – wounds of the chest;
- pathological – pathological process which developed in the wall or the chest;
- iatrogenic – as a consequence of medical interventions;
- spontaneous is when the blood is poured out in the pleural cavity spontaneously, the causes of this phenomenon are not installed.
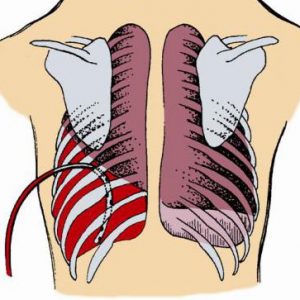

Iatrogenic hemothorax is actually kind of traumatic. Most often it occurs:
- after surgery – because of too extensive a forced trauma to the tissue, or if the bleeding was not stopped properly;
- during pleural puncture or thoracocentesisif they were performed with technical errors, or there were factors complicating the conduct;
- at the time of introduction of the catheter to a Central venous vessel.
Separately allocate the following forms of hemothorax:
- curdled – there is after surgery, when the patient according to testimony carried coagulant therapy (it aims to increase coagulation of blood – in particular, to prevent bleeding). Due to intake of coagulants of bleeding that got into the pleural cavity, collapsed faster than conventional hemothorax;
- pneumohemothorax in the pleural cavity accumulate at the same time blood and air. Observed in traumatic rupture of the lung, the melting hearth of tuberculosis and chest wound acute massive object.
Upon joining the infectious agent is isolated such forms of hemothorax:
- uninfected;
- infected. Often observed in the coagulated hemothorax when there is a rapid “settling” of intrapleural infection at a blood clot, and this, in turn, provokes subsequent purulent process – pyothorax (pus in the pleural cavity) or pleural empyema (purulent diffuse lesion of the pleural sheets).
A list of the most common cause of hemothorax is:
- wounds to the chest – often gunshot, stab, compression (if chest pressed heavy solid object);
- rib fractures (in an accident or is too intense cardiopulmonary resuscitation);
- aortic aneurysm;
- pulmonary tuberculosis;
- malignant neoplasms of the chest wall or the thorax (lung, pleura or the mediastinum), particularly in the stage of collapse;
- abscess of lung;
- the deterioration of the folding properties of the blood (occurs when coagulopathy, hemorrhagic diathesis, etc.).

The direct cause of hemothorax is a violation of the integrity of blood vessels:
- chest;
- easy.
Rarely bleeding occurs due to trauma of blood vessels of the mediastinum – thymus gland (or fatty tissue which it replaces), the part of the aorta outside of the heart shirts, trachea, esophagus, lymphatic ways and blood vessels and nerve structures. They are partially covered with light, which under the action of traumatic factors mainly take the brunt.
Hemothorax is often one-sided.
Bilateral lesion can sometimes be due to pronounced traumatisierung factors:
- at work (a fall from height);
- in case of accidents (in the accident);
- during natural disasters (collapses of the house);
- during military action;
- in sports (especially by force).
Bilateral hemothorax in 90-95% of cases means pronounced. It leads to the damage:
- intercostal arteries;
- aorta;
- Vena cava.
In these cases, the amount of blood that flows into the pleural cavity, can reach two liters and more. First, the diaphragmatic blood fills the pockets, but since the space of the pleural cavity is quite narrow, it is filled quickly, the blood begins to compress one or both lungs, due to which they cannot deal.
Signs of hemothorax
A small hemorrhage into the pleural cavity may not manifest clinically. This happens:
- when unexpressed pathological conditions of the chest wall and chest cavity, when corrupted by small vessels, and after the bleeding stopped spontaneously;
- because of the more pronounced symptoms that the pathological process which led to the development of the hemothorax and its drowns out the signs signs of hemorrhage.
Pronounced hemothorax is:
- clinical symptoms of respiratory;
- common features of the entire body.
Signs from the respiratory system:
- the feeling of pressure and heaviness in the chest. It can decrease if the patient lies on the affected side, or trying to take semi-sitting position in which blood flow allocation in the lower portions of the pleural cavity, pressure on lung tissue weakens;
- shortness of breath (rapid shallow breathing);
- the inability to inhale a full breast;
- the feeling of lack of air (due to the shutdown of the act of breathing compressed by the blood of lung segments);
- rapid breathing (to compensate for the feeling of shortage of air);
- bluish tint of the skin and visible mucous membranes. It is more pronounced and appears much faster than in hydrothorax, the same volume poured into the pleural cavity of fluid, as it will cause not only a deterioration in ventilation squeezed lung, but the bleeding;
- in the later stages of the infection – increased body temperature first up to subfebrile (37,0-37,3 degrees Celsius), and then higher, if developed purulent process in the form of pyothorax or empyema.
Common signs of acute blood loss, which occur when the hemothorax:
- pallor and then cyanosis of the skin and visible mucous membranes (in the case that compression of the lung manifested earlier than effects of the bleeding, pallor may not occur immediately fixed cyanosis);
- sweating, the sweat cold to the touch;
- hemodynamic changes (indicators characterizing the movement of blood through the vessels) – increased heart and pulse rate, hypotension.
Bilateral pneumothorax is regarded as extremely adverse condition. Even if both the pleural cavity initially poured out a small amount of blood, bleeding may recur and be more pronounced, which streamed with blood will be preloaded both lungs, and this will lead to decompensation of breath. Massive bilateral hemothorax death can occur in just a few minutes from its occurrence.
Complications hemorrhage into the pleural cavity
Are:
- early;
- late.
To early include:
- acute blood loss;
- compression (pinching) of the lungs by the blood, which leads to acute respiratory failure;
- the accession of infection and it “settling” on blood clot, which becomes an excellent breeding ground for microorganisms, resulting in advancing suppurative complications such as pyothorax or empyema. Infection blood discharge when hemothorax is regarded as a very unfavorable factor.
Late complications are:
- the formation of adhesions in the pleural cavity, which may hindered the movement of the diaphragm. In some cases the formation of adhesions can lead to a massive overgrowth of the lumen of the pleural cavity;
- respiratory insufficiency, which occurs most often because of adhesions in the pleural cavity.
The severity of complications depends on how severe was the bleeding into the pleural cavity.
When hemothorax distinguish four degrees of bleeding:
- low – blood loss of up to half a litre of blood accumulated in the sinuses (pockets) of the pleural cavity;
- average – in the pleural cavity was poured out to one and a half liters of blood, its level is determined lower than the fourth rib;
- Subtotal – blood loss is two liters, the blood level can go up to the second rib;
- total lost more than two liters of blood, she completely filled the pleural cavity and puts pressure on the lung from all sides.
A small but ongoing bleeding in many cases is more dangerous than a more pronounced, but stopped.
In this respect, there are two types of hemothorax:
- with a stable course;
- with increasing current.
Diagnosis
In the diagnosis of hemothorax rely on symptoms as manifestations from the respiratory system, and signs of bleeding.
But as a small hemorrhage in the pleural cavity may not manifest clinically, for diagnosis use additional methods of diagnosis:
- tool;
- lab.
In turn, the instrumental methods are:
- non-invasive (without the introduction into the pleural cavity);
- invasive (with the introduction).
For diagnosis of hemothorax following most informative non-invasive methods of instrumental examination of the patient:
The most affordable method and x-ray-graphy of the chest cavity. When hemothorax on the screen or the picture you can see the horizontal level of fluid in the pleural cavity (in some cases, increasing its quantity with continued bleeding). Clinical symptoms of bleeding will help to confirm that this fluid is the blood.
To invasive methods include:
- thoracentesis – chest wall and pleural covering it from the inside the leaf is pricked with a needle mounted on a syringe, and makes the suction motion to ensure that the pleural cavity has a bloody content;
- thoracocentesis – principle and tasks the same as when performing pleural puncture, but the puncture of the chest wall using a thicker than the needle, the device is a trocar, which is a tube with a sharp stiletto inside. When perforation with trocar chest wall it turns out the hole with a larger diameter than the puncture with a needle, through it is already possible to enter in the pleural cavity drainage tube;
- thoracoscopy is introduction of the thoracoscope into the pleural cavity, which can be used to identify the source of bleeding;
- rarely diagnostic thoracotomy, it is performed if other diagnostic methods it is impossible to establish the source of bleeding in the pleural cavity (e.g., in severe hemothorax). Often diagnostic thoracotomy in one examination is not the end – finding the source of bleeding, thoracic surgeons then performed the operation with the purpose of arresting bleeding.

In the diagnosis of hemothorax is used by such laboratory methods as:
- General blood analysis – changes (particularly the decrease in the number of erythrocytes and hemoglobin) to judge the severity of blood loss;
- sample Petrov – it can help identify loss of clarity of blood that flows into the pleural cavity, which indicates infection of the blood content.
- Proba Review-Gregoire – thanks to her determine the characteristics of blood clotting from the pleural cavity that will help to identify clotted hemothorax;
- cytological examination of sputum under a microscope – it will help to identify a disease that could cause of bleeding in the pleural cavity.
Emergency care and treatment of hemothorax
Therapeutic actions in case of hemothorax are divided into:
- first aid;
- treatment in a hospital.
If you suspect a hemothorax as first aid, should undertake the following steps:
- call the ambulance;
- to give the victim the situation with your head elevated;
- to the affected part of the chest (e.g., place of injury or the place to which the victim fell) to put cold ice, cold water in any capacity (if you do not have a suitable plastic bag, the water can be poured in a glass jar).
A patient with a hemothorax in a hospital environment is divided into:
- conservative;
- invasive.
Invasive methods of treatment, in turn, are divided into:
- puncture;
- operational.
Conservative therapy is aimed at:
- stopping bleeding (injected somehow prevent disease or to medications);
- renewal of circulating blood volume, which decreased as a result of bleeding into the pleural cavity (in the blood stream injected whole blood and blood components – fresh frozen plasma, erythrocyte mass, and the salt and protein solutions);
- preventing infection of the blood that flows into the pleural cavity (used antimicrobial agents of broad-spectrum and anti-inflammatory);
- the acceleration of resorption of blood in the pleural cavity (this makes injection of proteolytic enzymes – substances that can destroy proteins and injected them directly into the pleural cavity).
In more severe degrees of bleeding (particularly with symptoms of increasing respiratory distress) urgent evacuation of blood content from the pleural cavity.
This is performed using:
- pleural puncture;
- thoracocentesis.
These manipulations are carried out in the region of the sixth or seventh intercostal space along the back axillary line. Thoracentesis or thoracocentesis must be performed by the doctor. Blood is aspirated with a syringe or medical suction, the pleural cavity was washed with antiseptic, then she administered antimicrobials at the puncture site impose a sterile bandage.
If after pleural puncture or thoracocentesis the patient is not getting better, shows the urgent thoracotomy. Such an operation is:
- simple – between the ribs perform the incision through which penetrate into the pleural cavity. Is 7 or 8 intercostal space along the back axillary line;
- resection, perform the resection of the rib (partial removal). The length of the resected fragment is about three inches. This type of thoracotomy is resorted to, if the intercostal incision does not allow for adequate access to the pleural cavity. The patient should not worry about the resection of ribs – if you delete this small outline will appear no cosmetic defect or suffer the carcass of the chest.
With ongoing bleeding can be a open chestto get the technical ability to stop bleeding (ligation or plastics damaged blood vessels).
After stopping the bleeding in the pleural cavity is drained to enter one end of the drainage tube, the other is lowered into the liquid reservoir. Thus create a so-called siphon system, which allows blood to flow from the pleural cavity, but prevents a reverse current into the pleural cavity.
Surgical treatment should be accompanied by a conservative.
Prevention
The occurrence of hemothorax alert, avoiding dangerous situations that can lead to trauma of the thorax:
- household (fighting, diving in shallow water and falling from a height, especially such cases are more frequent during harvest from fruit trees);
- production (collapses in the mine);
- during large-scale natural disasters (earthquakes, tornadoes, tornadoes);
- during military actions.
If such injuries have arisen that need urgent consultation with thoracic surgeons who will promptly establish the fact of bleeding in the pleural cavity and will resort to actions that prevent the accumulation of blood fluid in the pleural cavity.
Alertness in respect of the hemothorax should be in the wounds of the abdomen.
Prevention of hemothorax is the prevention of diseases that can cause it in the first place is:
- aortic aneurysm;
- pulmonary tuberculosis;
- malignant tumors of the chest – especially at the advanced stage of decay.
So as not to cause iatrogenic hemothorax, manipulation of the rib cage (in particular, those that are blind, without a visual control – these include thoracentesis and thoracocentesis) you must perform very carefully and monitor if there is trauma to structures of the chest accompanied by bleeding. The same applies to thoracic surgery.
For the prevention of spontaneous hemothorax should be responsive to any pathological changes in the respiratory system and signs of internal bleeding. Quickly fixing it and taking hemostatic measures, you can prevent the accumulation of blood in the pleural cavity, which was caused causeless pleural bleeding.
Forecast
When intrapleural bleeding ranging from medium – degree forecast can be complex and depends on:
- the severity of the chest, in which there was a hemothorax;
- speed and duration of blood loss;
- timely diagnostic and therapeutic measures.
The prognosis for bilateral hemothorax is always difficult. Even if bleeding is slight, it is at any moment can become much more intense. As both of the affected half of the thorax, there will be decompensation of breath. The severity of the prognosis get worse with the form of clotted hemothorax. The most pessimistic projections – if the bilateral traumatic clotted hemothorax with ongoing bleeding.
It is more common in other varieties of hemothorax leads to:
- death;
- and if the patient survived – to long-term complications, for the relief of which require more time and more resources from both the patient and the physicians.
The prognosis is favorable if diagnosis and treatment of hemothorax was made in the first hours from the moment of its occurrence. After suffering a hemothorax forecast for health will be favorable in the case of correct rehabilitation of the patient.
To avoid late complications (formation of adhesions in the pleural cavity, impairing breathing), patients should begin to:
- regular practice of swimming;
- walking;
- special breathing exercises.
After suffering a hemothorax should be adjusted to what the recovery will be lengthy – sometimes required at least a year to finally get rid of the consequences of hemothorax.




It’s very easy to find out any matter on net as compared to books, as I found this article at this web site.
Gut geschrieben. Echt toll. Danke.
Sounds okay as an idea-quite possibly doomed to fail in reality, never mind eh?
I needed to compose you the little bit of note so as to thank you so much again just for the pretty views you have discussed in this case. It has been quite incredibly generous with people like you to grant extensively exactly what most of us might have sold as an ebook to help make some profit for their own end, and in particular considering the fact that you could possibly have tried it in case you desired. These pointers as well acted as a great way to recognize that the rest have a similar passion like mine to grasp a lot more with respect to this issue. I am certain there are lots of more enjoyable situations up front for individuals that browse through your site.