Anaerobic infection is an infectious process caused by the spore-forming or nonspore microorganisms under conditions favorable for their vital activity.
Characteristic clinical signs of anaerobic infections are prevalence of the symptoms of endogenous intoxication over local manifestations the putrid character of the exudate, gas-forming processes in the wound, rapidly progressive tissue necrosis.
Anaerobic infection is recognized on the basis of clinical findings, supported by results of microbiological diagnostics, gas chromatography, mass spectrometry, immunoelectrophoresis, PCR, ELISA, etc. Treatment of anaerobic infections involves radical surgical processing of purulent focus, intense antibacterial and detoxication therapy.
Anaerobic infection
Anaerobic infection – the pathological process, causative agents of which are anaerobic bacteria, developing in conditions of anoxia (lack of oxygen) or hypoxia (low oxygen tension).
Anaerobic infection is a severe form of infectious process, accompanied by the defeat of vital organs and high mortality rate. In clinical practice, with anaerobic infection faced by the experts in the field of surgery, traumatology, Pediatrics, neurochirugie, otolaryngology, dentistry, pulmonology, gynecology, and other medical areas.
Anaerobic infection may occur in patients of any age. The proportion of diseases caused by anaerobic infection is not exactly known; purulent foci of soft tissue, bones or joints anaerobes are sown about 30% of cases; anaerobic bacteremia is confirmed in 2-5% of cases.
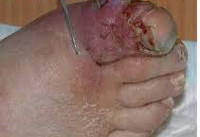
Causes and characteristics of anaerobic infections
Anaerobes are part of normal microflora of the skin, mucous membranes, gastrointestinal tract, urogenital organs and their virulent properties are opportunistic. Under certain conditions, they become pathogens of endogenous anaerobic infections. Exogenous anaerobic bacteria are present in soil and decomposing organic masses and cause the disease process when injected into the wound from the outside. Anaerobic microorganisms are divided into obligatory and elective: development and reproduction of obligate anaerobes is carried out in an oxygen-free environment; facultative anaerobes can survive both in the absence and in the presence of oxygen. Facultative anaerobic bacteria belong to the Escherichia coli, Shigella, Yersinia, Streptococcus, Staphylococcus etc.
Obligate pathogens anaerobic infections are divided into two groups: spore-forming (Clostridium) and nonspore (non-clostridial) anaerobes (fuzobakterii, Bacteroides, veillonella, Propionibacterium, Peptostreptococcus, etc.). Spore-forming anaerobes are the causative agents of clostridial exogenous origin (tetanus, gas gangrene, botulism, food poisoning, etc.). Non-clostridial anaerobes in most cases, the cause of purulent-inflammatory processes of endogenous nature (abscesses of internal organs, peritonitis, pneumonia, cellulitis of the maxillofacial region, otitis media, sepsis, etc.).
The main virulence factors of anaerobic microorganisms serve their number in the pathological focus, biological properties of pathogens, the presence of bacterial associates are realized. In the pathogenesis of anaerobic infections leading role produced by microorganisms enzymes, endo – and exotoxins, nonspecific factors of metabolism. Thus, the enzymes (heparinase, hyaluronidase, collagenase, DNase) is able to enhance the virulence of anaerobes, destruction of muscle and connective tissue. Endo – and exotoxins cause damage to the vascular endothelium, intravascular hemolysis and thrombosis. In addition, some clostridial toksiny have nephrotropic, neurotropic, cardiotropic action. Also the toxic effect on the body have and nonspecific factors of metabolic anaerobes – indole, fatty acids, hydrogen sulfide, ammonia.
The conditions conducive to the development of anaerobic infection is a damage to anatomical barriers penetration of anaerobic bacteria in the tissue and blood stream, and also decrease the redox potential of the tissues (ischemia, hemorrhage, necrosis). The penetration of anaerobic bacteria in tissue can occur during surgical interventions, invasive manipulation (puncture, biopsy, tooth extraction, etc.), perforation of internal organs, open injuries, wounds, burns, animal bites, crush syndrome, criminal abortion, etc. Factors contributing to the emergence of anaerobic infections, massive pollution of the land, the presence of foreign bodies in the wound, hypovolemic and traumatic shock, concomitant diseases (collagenosis, diabetes mellitus, tumors), immunodeficiency. In addition, great importance is irrational antibiotic therapy aimed at the suppression of the accompanying aerobic flora.
Depending on localization distinguish anaerobic infection:
- Central nervous system (brain abscess, meningitis, subdural empyema, etc.)
- head and neck (periodontal abscess, Ludwig’s angina, otitis media, sinusitis, cellulitis of the neck, etc.)
- respiratory tract and pleura (aspiration pneumonia, lung abscess, empyema, etc.)
- the female reproductive system (bartholinitis, salpingitis, adnexitis, endometritis, pelvioperitonit)
- the abdomen (abdominal abscess, peritonitis)
- skin and soft tissue (clostridial cellulitis, gas gangrene, necrotizing fasciitis, abscissae etc.)
- bones and joints (osteomyelitis, purulent arthritis)
- the bacteremia
The symptoms of anaerobic infections
Regardless of the type of pathogen and localization of anaerobic infection of different clinical forms are characterized by some common features. In most cases, anaerobic infection has an acute onset and is characterized by a combination of local and General symptoms. The incubation period can vary from several hours to several days (average 3 days).
A typical feature of anaerobic infections is the prevalence of symptoms of intoxication on the local inflammatory phenomena. The sharp deterioration in the General condition of the patient usually occurs before the appearance of local symptoms. A manifestation of severe endotoxemia is a high fever with chills, extreme weakness, nausea, headache, confusion. Characteristic arterial hypotension, tachypnea, tachycardia, hemolytic anemia, ikterichnost skin and sclera, acrocyanosis.
When wound anaerobic infection early local symptom is very strong, increasing pain expander nature, emphysema and crepitus soft tissues caused by gas-forming processes in the wound. Among the permanent features include aharony fetid odor of exudate, associated with the excretion of nitrogen, hydrogen and methane by anaerobic oxidation of the protein substrate. The exudate is liquid, serous, hemorrhagic, purulent, hemorrhagic or purulent in nature, heterogeneous in color, interspersed with fat and the presence of gas bubbles. On the rotten nature of inflammation also indicates the appearance of a wound that contains tissue gray-green or gray-brown, sometimes scabs in black.
For anaerobic infection can be lightning fast (within 1 day after surgery or injury), acute (within 3-4 days), subacute (more than 4 days). Anaerobic infection is often accompanied by the development of multiple organ failure (hepatic, renal, cardiopulmonary), infectious-toxic shock, severe sepsis, causing death.
Diagnosis of anaerobic infection
For timely diagnosis of anaerobic infections is of great importance a correct assessment of clinical symptoms, allowing time to provide the necessary medical care. Depending on the localization of the infectious focus with the diagnosis and treatment of anaerobic infections can engage clinicians of various specialties – General surgery, trauma surgeons, neurosurgeons, gynecologists, otolaryngologists, maxillofacial, and thoracic surgeons.
The methods of Express diagnostics of anaerobic infections include a wound with bacterioscopy color smear by Gram and gas-liquid chromatography. In the verification of the pathogen leading role of bacteriological seeding detachable wounds or contents of the abscess, analysis of pleural fluid, blood culture for aerobic and anaerobic bacteria, immune-enzyme analysis, PCR. In the biochemical blood parameters in anaerobic infections detected by a decrease in the concentration of proteins, increase the level of creatinine, urea, bilirubin, transaminases and alkaline phosphatase. Along with clinical and laboratory tests, performs x-rays, which revealed the accumulation of gas in the affected tissues or cavities.
Anaerobic infection should be differentiated from erysipelas of soft tissue, a polymorphic exudative erythema, deep vein thrombosis, pneumothorax, pneumoperitoneum, perforation of hollow abdominal organs.
Treatment of anaerobic infections
A comprehensive approach to the treatment of anaerobic infections involves carrying out radical surgical processing of purulent focus, intense detoxification and antibiotic therapy. Surgical stage should be done as early as possible – depends on the patient’s life. As a rule, it consists in a wide dissection of the lesion with removal of necrotic tissue, decompression of the surrounding tissues, open drainage with lavage of the cavities and wounds with antiseptic solutions. Peculiarities of anaerobic infections often require additional necrectomy, disclosure of purulent pockets, the treatment of wounds with ultrasound and laser, ozone therapy, etc. With extensive destruction of tissue may be indicated amputation or disarticulation of a limb.
The most important components of the treatment of anaerobic infection are intense fluid therapy and antibiotic medication broad-spectrum, vysokoduhovnym to anaerobes. In the framework of complex treatment of anaerobic infection find its application of hyperbaric oxygenation, UFOC, extracorporeal (hemosorption, plasmapheresis, etc.). If necessary, the patient is protivogangrenoznaya antitoxic serum.
Prognosis and prevention of anaerobic infections
The outcome of anaerobic infection depends largely on the clinical forms of pathological process, premorbid background, the timeliness of diagnosis and initiation of treatment. The fatality rate in some forms of anaerobic infection exceeds 20%. Prevention of anaerobic infections is a timely and adequate PHO wounds, removal of foreign bodies soft tissues, compliance with the requirements of asepsis and antisepsis in operations. Wound with extensive damage and high risk of development of anaerobic infections is necessary to conduct specific immunization and antimicrobial prophylaxis.



Outstanding post, I think blog owners should acquire a lot from this website its really user friendly.
Thanks for your text. I would also love to say a health insurance brokerage also works best for the benefit of the coordinators of your group insurance cover. The health insurance professional is given a long list of benefits sought by someone or a group coordinator. What a broker really does is try to find individuals and also coordinators which usually best go with those needs. Then he provides his advice and if all sides agree, the particular broker formulates legal contract between the two parties.
I have been exploring for a little bit for any high quality articles or blog posts on this kind of space . Exploring in Yahoo I ultimately stumbled upon this site. Reading this information So i’m happy to convey that I’ve a very excellent uncanny feeling I discovered exactly what I needed. I so much indubitably will make certain to don’t put out of your mind this web site and give it a glance regularly.
Nice post. I learn something more challenging on different blogs everyday. It will always be stimulating to read content from other writers and practice a little something from their store. I?d prefer to use some with the content on my blog whether you don?t mind. Natually I?ll give you a link on your web blog. Thanks for sharing.
some genuinely grand work on behalf of the owner of this site, perfectly great subject matter.
Totally DUG this post! I have a blog myself, if you are open, I might curate this post to my audience. Obviously give a link back.
Please let me know if you’re looking for a author for your weblog. You have some really great articles and I feel I would be a good asset. If you ever want to take some of the load off, I’d really like to write some material for your blog in exchange for a link back to mine. Please send me an e-mail if interested. Kudos!
I have read a few good stuff here. Definitely worth bookmarking for revisiting. I wonder how much effort you put to create such a wonderful informative site.
Excellent post. I used to be checking continuously this weblog and I am impressed!
Extremely useful info particularly the closing section :
) I take care of such information much. I used to be looking for this particular information for a
very long time. Thank you and good luck.