A toddler has become the first person in the UK to have a pig-skin transplant.
Two-year-old Eve Phillipson, from Doncaster, underwent five-hour surgery to create an artificial diaphragm containing the animal’s hide.
The youngster, who was diagnosed with Congenital Diaphragmatic Hernia (CDH) while still in the womb, was not expected to live after earlier transplants failed.
In a ground-breaking procedure, two of the three muscles in Eve’s abdominal wall were turned to create a natural diaphragm. Medically-sterilised pig skin, known as Strattice, was then used to reinforce the weakness in the wall.
Although the youngster still requires constant ventilation and oxygen, Eve’s successful operation has lead to her being hailed ‘a little ray of hope’ for others with the same condition.
Despite the challenges she faces, Eve’s mother Rebecca, 38, insists her ‘playful’ daughter is as happy as any other two-year-old.
CDH affects one in every 10,000 newborns. It occurs when a hole develops in the muscle that separates the chest from the stomach, causing organs to enter the thorax and squash the lungs.
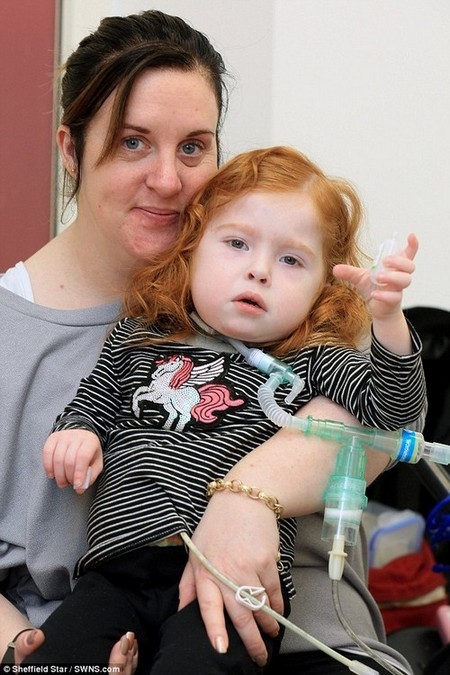
Eve Phillipson (pictured with her mother Rebecca, 38), two, is the first person in the UK to have a pig-skin transplant after having an artificial diaphragm created from the animal’s hide
Two of the three muscles in Eve’s abdominal wall were turned to create a natural diaphragm. Medically-sterilised pig skin was then used to reinforce the weakness in her abdominal wall
The operation was successful with Rebecca describing her daughter as ‘playful’ and ‘funny’
Born without a diaphragm
While most CDH sufferers have small holes in their diaphragms, Eve was missing the organ altogether, leading to her requiring immediate life support after she was born.
Rebecca said: ‘We went to our 12 week scan and she had more fluid than normal on the back of her neck, so they scanned Eve again at 15 weeks and found the CDH.’
Eve first underwent surgery to replace her missing diaphragm when she was just one-week-old.
Unfortunately, the artificial implant was unsuccessful and Eve’s health started to decline as she grew older.
Rebecca said: ‘By her second birthday we were concerned that if we didn’t go for the ground-breaking surgery to create a natural diaphragm, we might lose her.’

Despite her surgery being successful, Eve still requires constant ventilation and oxygen
Rebecca says her daughter is ‘a ray of hope’ for others who are battling the same condition
Eve was given a 50:50 survival chance, which her mother said was ‘an emotional rollercoaster’
‘A little ray of hope’
Consultant Paediatric Surgeon Sean Marven, who carried out the procedure at the Sheffield Children’s NHS Foundation Trust, said: ‘It was a very difficult decision. We knew the longer we waited, the more perilous the procedure may be.
‘The surgery was complex and required a great deal of skill and concentration, particularly as it had never been performed in the UK before.
‘Thankfully it went well and Eve continues to grow stronger’.
Due to Eve suffering a collapsed left lung as a result of her condition, she still requires ventilation support.
Her family hope she will be able to live without such support in the future, but insist she is still like any other toddler.
Rebecca said: ‘She smiles, she plays, she’s mischievous, she’s funny; what more can you ask for than that?
‘It will be nice when we get her off the ventilator and off oxygen, but we’ll get there when we get there.
‘If other families are going through a dark time, Eve can be a little ray of hope for them. Sometimes even the worst cases can turn out well’.
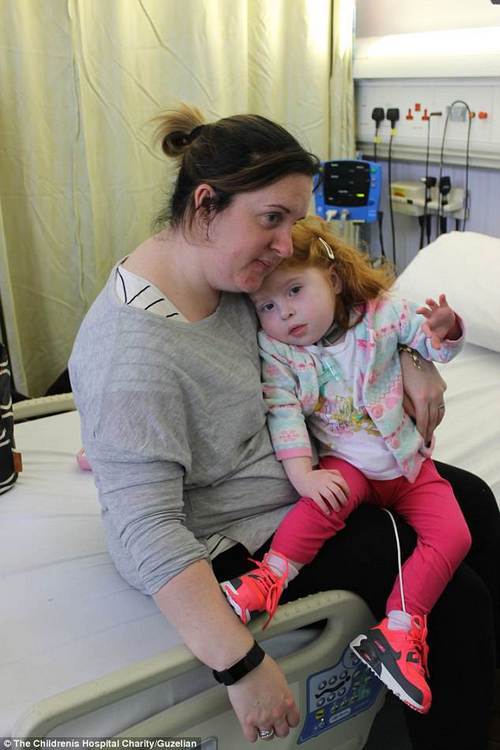
After being diagnosed in the womb, Eve’s health deteriorated when her first transplant failed
Surgeons performed the ‘perilous’ procedure, anxious she would only get worse with age
‘It was an emotional rollercoaster’
The Children’s Hospital Charity, which funded Eve’s operation, is also backing research to improve the information provided to surgeons and parents during pregnancies where CDH is suspected.
Speaking of her own experience, Rebecca said: ‘It was quite overwhelming. We were told she had a 50:50 chance of survival and we didn’t know the extent of the damage until she was born.
‘It was an emotional rollercoaster and an incredibly anxious time’.
The research project uses an MRI scan taken during routine pregnancy ultrasounds to create 3D animations of the unborn baby and their individual CDH.
This helps surgeons see the extent of any damage, which then allows them to choose the best type of operation to treat patients. The images would also be provided to parents to help ease their anxiety.
The study forms part of The Children’s Hospital Charity’s annual commitment to spend up to £250,000 on research into the prevention and cure of childhood illnesses.
Lead researcher, Dr Elspeth H Whitby, senior lecturer at the University of Sheffield, said: ‘The project wouldn’t have been possible without funding from The Children’s Hospital Charity.
‘The research will help families and patients at Sheffield Children’s Hospital, but it will also benefit any family dealing with CDH in Yorkshire and could be implemented nationwide if successful’.
David Vernon-Edwards, The Children’s Hospital Charity’s director, added: ‘As a charity we are very proud to play an important role in ensuring that innovative research continues to be funded, helping children to get better and lead full lives. Eve’s incredible resilience is an inspiration to us all’.
To find out more about this research project and others funded by The Children’s Hospital Charity here.

Rebecca believes Eve’s inspiring story shows ‘even the worst cases can turn out well’
Her mother is anxious for Eve to come off her ventilator but says it will happen when it happens
Despite her health challenges, Rebecca insists Eve is as happy as any other two-year-old