Arthrocentesis (synovial fluid aspiration) can be performed diagnostically (for identification of the etiology of acute arthritis) or therapeutically (for pain relief, drainage of effusion, or injection of medications).
The clinician performing the procedure should be familiar with the anatomy of the specific joint in order to avoid puncture of tendons, blood vessels, and nerves.
Using the extensor surface of the joint for needle insertion, while keeping the joint in minimal flexion, minimizes the risk of such injuries.
Background
The ankle joint is a hinged synovial joint with primarily up-and-down movement (plantarflexion and dorsiflexion). However, when the ranges of motion (ROMs) of the ankle and subtalar joints (talocalcaneal and talocalcaneonavicular) are taken together, the complex functions as a universal joint. For more information about the relevant anatomy, see Ankle Joint Anatomy.
Indications
Diagnostic indications for ankle arthrocentesis include the following:
-
Evaluation of monoarticular arthritis
- Evaluation of suspected septic arthritis
- Evaluation of joint effusion
- Identification of intra-articular fracture
- Identification of crystal arthropathy
Therapeutic indications include the following:
- Relief of pain by aspirating effusion (including hemarthrosis)
- Injection of medications (eg, corticosteroids, antibiotics, anesthetics)
- Drainage of septic effusion
Contraindications
There are no absolute contraindications for ankle arthrocentesis.
Relative contraindications include the following:
-
Suspected septic joint – In this case, no contraindications exist
- Cellulitis overlying the joint – If arthrocentesis is performed, the patient should be admitted for intravenous antibiotics, even if the synovial fluid is not suspicious for infectious arthritis
- Skin lesion or dermatitis overlying the joint
- Known bacteremia
- Adjacent osteomyelitis
- Uncontrolled coagulopathy
- Joint prosthesis – Preferably, a joint prosthesis is tapped by an orthopedist
Periprocedural Care
Equipment
Equipment used for ankle arthrocentesis includes the following:
-
Sterile gloves and drapes
- Gauze pads (5), 4 × 4 in.
- Skin preparatory solution
- Lidocaine 1%
- Syringe, 5 mL
- Needles, 18 gauge and 25 or 27 gauge
- Syringes, 20 mL, 30 mL, 60 mL
- Needle, 18 gauge or 20 gauge (a patient who is morbidly obese might require a 21-gauge spinal needle for arthrocentesis)
- Hemostat
- Specimen tubes
- Bandage
Patient Preparation
Anesthesia
Patients who are anxious, in severe pain, or unable to cooperate with the procedure might require procedural sedation and/or analgesia. For more information, see Procedural Sedation.
Local anesthesia is warranted. After skin preparation, draping, and identification of the needle insertion site, use a 25- or 27-gauge needle to inject 2-5 mL of local anesthetic (eg, lidocaine 1%) into the subcutaneous tissue. (See the image below.) For more information, see Local Anesthetic Agents, Infiltrative Administration.
Infiltration of local anesthetic.
Deep injections that might enter the joint space are not recommended, because they may alter the synovial fluid analysis results.
Positioning
The patient should be placed either sitting or supine on a stretcher, with the knee flexed at 90º and the leg either hanging from the side of the stretcher or bent with the heel resting against the stretcher.
Plantarflexion of the ankle against minimal ankle dorsiflexion by the patient helps define the anatomy.
Technique
Aspiration of Synovial Fluid From Ankle
Prepare the skin with sterile solution, allow drying, and then drape.
Using a sterile technique, attach the 18- or 20-gauge needle to the 20-mL syringe, and pull the plunger to break resistance.
While stretching the skin over the insertion site (see below for choices of insertion site), insert the needle into the joint space while gently aspirating until synovial fluid enters the syringe (usually 1-2 cm in an adult of average size). If a bone is encountered, pull the needle back, verify the anatomic landmarks (see the images below), and readvance the needle in a corrected direction.
If removal of more fluid is desired, a hemostat flush to the skin can be used to secure the needle in place while the syringe is replaced with a new one.
Remove the needle and apply a bandage.
Divide the aspirated synovial fluid into the different specimen containers.
Anterolateral approach (preferred)
This is the preferred approach for ankle joint aspiration because it avoids potential injury to the dorsalis pedis and posterior tibial vessels or the deep peroneal nerve, which course through the medial aspect of the ankle and foot.
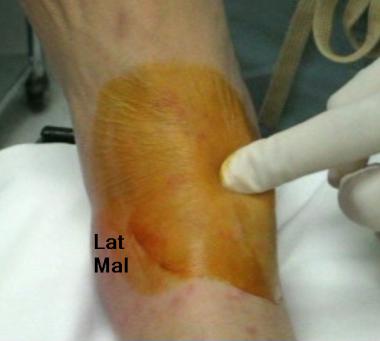
Identify the ankle joint line, the lateral malleolus, and the lateral border of the extensor digitorum longus (EDL).
Extension of the foot against the patient’s resistance or active flexion/extension movement by the patient helps the practitioner identify the space between the base of the lateral malleolus and the lateral border of the EDL.
Insert a needle (18-20 gauge) at the joint line midway between the base of the lateral malleolus and the lateral border of the EDL, advancing the needle perpendicular to the fibular shaft.
Anteromedial approach
Exercise care with this approach to avoid injury to both the dorsalis pedis vessels and the deep peroneal nerves that are immediately below and lateral to the extensor hallucis longus (EHL) tendon.
Identify the ankle joint line, the medial malleolus, and the tendons of the EHL and the tibialis anterior.
Extension of the foot against the patient’s resistance or active flexion/extension movement by the patient helps the practitioner identify the space between the medial border of the EHL and the lateral border of the tibialis anterior or between the base of the medial malleolus and the medial border of the tibialis anterior. (See the image below.)
Identification of space between medial malleolus and medial border of tibialis anterior tendon.
Insert a needle (18-20 gauge) at either insertion point, and advance the needle perpendicular to the tibial shaft. (See the image below.)
Ankle joint aspiration between medial malleolus and medial border of tibialis anterior tendon.
Analysis of Synovial Fluid
The aspirated synovial fluid is then analyzed (see Table 1 below).8
Table 1. Synovial Fluid Analysis in Different Diseases (Open Table in a new window)
| Appearance | WBC, cells/μL | Polymorphonuclear (PMN) cells, % | Glucose concentration, mg/dL | Protein concentration, g/dL | |
| Normal | Clear | <150 | <0.25 | Serum glucose | 1.3-1.8 |
| Noninflammatory | Clear | <3000 | <0.25 | Serum glucose | 2-3.5 |
| Inflammatory | Cloudy | >3000 | <0.75 | <25 | >4 |
| Purulent | Cloudy | >50,000 | >0.9 | <25 | >4 |
| Hemorrhagic | Bloody | >2000 | ~0.3 | Serum glucose | … |
Operative characteristics of septic joint effusion findings include the following:
-
Total white blood cell (WBC) count >25,000/μL (sensitivity, 77%; specificity, 73%; positive likelihood ratio LR +, 29; negative likelihood ratio LR –, 0.71)
- Total WBC count >50,000/μL (sensitivity, 62%; specificity, 92%; LR +, 7.7; LR –, 0.42) 9
- Total WBC count >100,000/μL (sensitivity, 22%; specificity, 99%; LR +, 2.9; LR –, 0.32)
- PMN cells ≥90% (sensitivity, 73%; specificity, 79%; LR +, 3.4; LR –, 0.34)
- Synovial glucose or serum glucose concentration <0.5 mg/dL (sensitivity, 51%; specificity, 85%; LR +, 3.4; LR –, 0.58)
- Protein concentration >3 g/dL (sensitivity, 48%; specificity, 46%; LR +, 0.9; LR –, 1.1)
- Lactic dehydrogenase (LDH) concentration >250 U/L (sensitivity, 100%; specificity, 51%; LR +, 1.9; LR –, 0.1)
Although uncommon, crystal-induced arthritis and septic arthritis can coexist; therefore, the presence of crystals does not exclude bacterial arthritis.10
Complications
Improper needle placement, a small amount of effusion, mechanical obstruction of the needle against cartilage, or thickened synovium can result in a dry tap.
Potential damage to cartilage can be avoided by understanding the joint anatomy and avoiding further advancement of the needle into the joint space once synovial effusion enters the syringe.
Most hemarthroses are small and self-limited and only require observation. Hemarthrosis in coagulopathic patients may require correction of the coagulopathy after consideration of the relative risks of reversal. Proper skin cleansing and use of aseptic technique reduces the risk of introducing infection into a sterile joint to less than 1:10,000.
When performing arthrocentesis through infected skin for the diagnosis of a potentially septic joint, intravenous antibiotics should be given immediately following the procedure, and the patient should be admitted for continuation of the antibiotics.
References
- Siva C, Velazquez C, Mody A, Brasington R. Diagnosing acute monoarthritis in adults: a practical approach for the family physician. Am Fam Physician. 2003 Jul 1. 68(1):83-90. Medline. Full Text.
- Tallia AF, Cardone DA. Diagnostic and therapeutic injection of the ankle and foot. Am Fam Physician. 2003 Oct 1. 68(7):1356-62. Medline. Full Text.
- Lenhard A, Moallem M, Marrie RA, Becker J, Garland A. An intervention to improve procedure education for internal medicine residents. J Gen Intern Med. 2008 Mar. 23(3):288-93. Medline.
- Sack K. Monarthritis: differential diagnosis. Am J Med. 1997 Jan 27. 102(1A):30S-34S. Medline.
- Margaretten ME, Kohlwes J, Moore D, Bent S. Does this adult patient have septic arthritis?. JAMA. 2007 Apr 4. 297(13):1478-88. Medline.
- Chen LX, Schumacher HR. Current trends in crystal identification. Curr Opin Rheumatol. 2006 Mar. 18(2):171-3. Medline.
- Dooley P, Martin R. Corticosteroid injections and arthrocentesis. Can Fam Physician. 2002 Feb. 48:285-92. Medline.
- Margaretten ME, Kohlwes J, Moore D, Bent S. Does this adult patient have septic arthritis?. JAMA. 2007 Apr 4. 297(13):1478-88. Medline.
- McGillicuddy DC, Shah KH, Friedberg RP, Nathanson LA, Edlow JA. How sensitive is the synovial fluid white blood cell count in diagnosing septic arthritis?. Am J Emerg Med. 2007 Sep. 25(7):749-52. Medline.
- Ungprasert P, Kaewpoowat Q, Ratapano S, Srivali N, Bischof EF Jr. Presence of crystals is not an evidence of absence of infection. Am J Emerg Med. 2013 Feb. 31(2):455.e1-2. Medline.




Thanks for the suggestions you discuss through this site. In addition, many young women who seem to become pregnant never even try to get health insurance because they are concerned they might not qualify. Although a few states now require that insurers offer coverage despite the pre-existing conditions. Fees on all these guaranteed programs are usually larger, but when with the high cost of health care bills it may be some sort of a safer strategy to use to protect one’s financial potential.