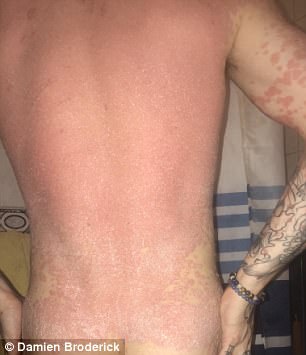
Electroshock therapy delivers pulses of electricity to the brain through electrodes to treat depression, and new research suggests more patients should try it sooner.
A modern form of electric shock therapy should be used to treat depression in more patients, and sooner, a new study’s findings suggest.
Once feared, reviled and even labelled as torture, shock therapy has come a long way, technologically. Though it has shown great promise for tough-to-treat cases of depression, it is still very rarely utilized.
The far safer modern form of shock therapy could effectively treat half of patients that drugs and talk therapy failed, sparing them years of depression and costs, according to the University of Michigan researchers.
Shock therapy – more accurately called electroconvulsive therapy (ECT) – was introduced in the 1930s as a treatment for various mental illnesses.
The treatment has a troubled history of abuse, but in its modern form, it has been a singular source of relief for patients with difficult-to-treat cases of depression, like that of the late actress Carrie Fisher.

ECT induces a seizure by delivering pulses of electricity to the brain. Before the treatment was invented in Italy, psychiatrists could achieve the same thing using a drug called Metrazol.
Patients reported that the drug gave them a feeling of sheer terror as it kicked in, just before a seizure began. ECT was supposed to be a less traumatic substitute. Doctors all around the world quickly adopted ECT and many patients received unprecedented relief from their psychiatric symptoms.
But there was a dark side to the new therapy.
For the first 20 years of the practice, ECT was delivered to patients while they were awake, and often using a higher voltage shocks. As a result, patients would often thrash violently as they seized, sometimes injuring themselves.
In addition to physical injuries, there were reports that many mental institutions would threaten misbehaving patients with shock therapy as a means of control.
This abusive practice was famously immortalized in the 1975 film One Flew Over The Cuckoo’s Nest, when Jack Nicholson’s rebellious character is hauled off by cruel staff members at a mental institution, strapped to a table and shocked into submission.
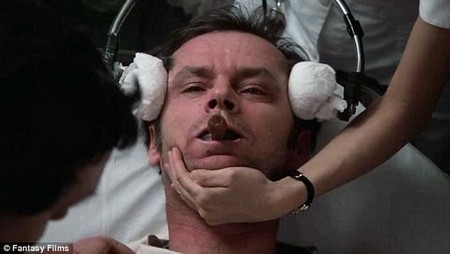
The treatment was once abused by psychiatrists in mental institutions who threatened patients with it, as portrayed in One Flew Over The Cuckoo’s Nest. The horrifying scene solidified shock therapy’s reputation as more of a torture method than a treatment, but is not representative of today’s ECT.
Now, patients are typically get a muscle relaxer before ECT, and are put under anesthesia for the duration of the procedure. Doctors closely monitor their brain waves to make sure they electrical pulses are not overly distressing the brain and watching for the seizure activity they aim to induce.
There typically are not any actual convulsions for the modern patient. A seizure induced by electrical shocks can act as a sort of reset for the brain, changing patterns of activity and blood flow.
For some patients – including the late actress Carrie Fisher – it seems to be the only thing that does work to treat mental illnesses like depression. ECT is used as a treatment of last resort – and only for a very small minority of patients in the US.
The late Star Wars actress Carrie Fisher swore by ECT to treat her persistent depression. An estimated 100,000 Americans get ECT each year.
But that is barely a drop in the proverbial bucket of the 3.3 million people who struggle with depression, 67 percent of whom get some form of treatment. The University of Michigan researchers reviewed recent literature on the use of electroshock therapy.
Analyzing data on veterans who had been treated for depression, they found that only 0.16 percent had been given ECT – and for most of them it was a fourth, fifth or even seventh line of treatment.
Yet conservative estimates put its effectiveness at about 50 percent, while the first antidepressant drug they tried worked for only a third or patients, with returns diminishing with each additional drug they were prescribed.
‘Unfortunately, research shows that with multiple medication failures and long duration of illness – sometimes many years – the chance that patients can achieve remission drops quickly to very low numbers,’ said senior author Dr Daniel Maixner.
On the other hand, he said: ‘ECT is the best treatment to produce remission,’ which it did for many patients, immediately and fully, with some relapses after a year.
At first blush, ECT is more expensive than drug treatments, costing about $2,500 per session.
But after examining cost and quality of life data, the University of Michigan team concluded that ECT would actually save patients money if it was used as a third-line treatment, instead of a continuing cycle of different medications.
‘In addition to the clinical idea that ECT should be used sooner, our study adds another perspective highlighting that ECT is also cost-effective earlier in the treatment course of depression,’ said Dr Maixner.