Patients with complicated aortic aneurysms are urgently hospitalized in the cardiac surgery department. Conservative therapy is indicated for any form of the disease at the initial stage of treatment in order to stop the progression of the vascular wall bundle and stabilize the patient’s condition.
Intensive therapy of dissecting aortic aneurysm is aimed at relieving pain syndrome (by administering non-narcotic and narcotic analgesics), removing from the shock, reducing blood pressure.
Hemodynamics, heart rate, diuresis, CVP, pulmonary artery pressure are monitored. With clinically significant hypotension, it is important to quickly restore BCC due to intravenous infusion of solutions.
Drug treatment is essential in most patients with uncomplicated dissecting aneurysms of type B (with distal dissection), with a stable isolated separation of the aortic arch and stable uncomplicated chronic dissection. With the ineffectiveness of the therapy, the progression of the bundle and the development of complications, as well as patients with acute proximal aortic wall dissection (type A) immediately after stabilization of the condition, emergency surgical intervention is shown.
In case of dissecting aortic aneurysm, resection of the aorta damaged area is performed with anguish, removal of the intimate flap, elimination of the false lumen and restoration of the excised aortic fragment (sometimes a one-time reconstruction of several branches of the aorta) using a prosthetic technique or approaching ends. In most cases, the operation is performed under conditions of artificial blood circulation. According to the indications, valvuloplasty or aortic valve replacement, reimplantation of the coronary arteries is performed.
Dissecting aortic aneurysm – a defect in the inner lining of the aneurysmally expanded aorta, accompanied by the formation of a hematoma, longitudinally dissecting the vascular wall with the formation of a false channel. Dissecting aortic aneurysm is manifested by sudden intense pain migrating along the course of dissection, an increase in blood pressure, signs of ischemia of the heart, brain and spinal cord, kidneys, internal bleeding. The diagnosis of vascular wall dissection is based on EchoCG, CT and MRI of the chest / abdominal aorta, aortography. Treatment of a complicated aneurysm includes intensive drug therapy, resection of the damaged area of the aorta, followed by reconstructive plasty.
Dissecting aortic aneurysm – longitudinal separation of the aortic wall in the distal or proximal direction at different lengths, due to the rupture of its inner membrane and the penetration of blood into the thickness of the degenerative-modified middle layer. Expansion of the aorta during exfoliation of its wall may be moderate or absent, so dissecting aortic aneurysm is often called aortic dissection.
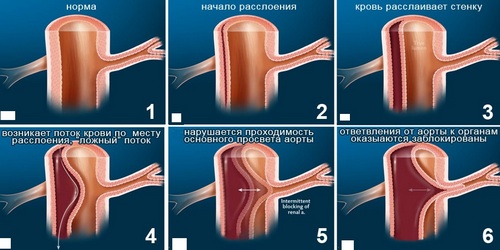
Most aneurysms are localized in the most hemodynamically vulnerable areas of the aorta: about 70% in the ascending part a few centimeters from the aortic valve, 10% of cases in the arch, 20% in the descending aorta distal to the mouth of the left subclavian artery.
Dissecting aneurysm in cardiology refers to life-threatening conditions with the risk of massive bleeding with aortic rupture or acute ischemia of vital organs (heart, brain, kidneys, etc.) during occlusion of the main arteries. Usually, aortic aneurysm dissection occurs at the age of 60-70 years, in men 2-3 times more often than in women.
Causes of dissecting aortic aneurysm
The causes of pathology are diseases and conditions that lead to degenerative changes in the muscular and elastic structures of the middle aortic membrane (media). The main risk of aortic dissection is associated with prolonged arterial hypertension (70-90% of cases), accompanied by hemodynamic stress and chronic aortic trauma.
Dissecting aneurysm can develop as a complication of hereditary connective tissue defects (Marfan, Turner, Ehlers-Danlos syndromes), aortic defects, aortic coarctation, marked aortic atherosclerosis, systemic vasculitis, polycystic kidney disease. Elderly patients (older than 60-70 years), chest injuries, III trimester of pregnancy in women older than 40 years are considered risk factors for aortic aneurysm dissection.
In the early and late postoperative period after surgical interventions on the heart and aorta (aortic valve replacement, aortic resection), there is an increased risk of aneurysm dissection. Iatrogenic dissecting aneurysms are associated with technical errors when performing aortography and balloon dilatation, cannulation of the aorta to provide artificial blood circulation.
The primary pathogenetic link in most cases is an intimal tear, followed by the formation of an intraparietal hematoma. In about 10% of cases, dissecting an aortic aneurysm can initiate bleeding in the media during spontaneous rupture of capillaries branching out in the aortic wall. The spread of intramural hematoma within the media is usually accompanied by a subsequent intimal rupture, but can occur without it (in 3-13% of cases). In rare cases, aortic dissection can be observed when an atherosclerotic ulcer penetrates.
Classification of dissecting aortic aneurysm
According to the DeBakey classification, 3 types of delamination are determined:
- I – an intimal tear in the ascending segment of the aorta, the dissection extends to the thoracic and abdominal parts;
- II – the place of anguish and dissection is limited to the ascending aorta,
- III – tearing of the intima in the descending aorta, the dissection can spread to the distal parts of the abdominal aorta, sometimes retrograde to the arch and the ascending part.
The Stanford classification distinguishes A-type dissecting aortic aneurysms, with proximal dissection affecting its ascending division, and type B with distal dissection of the arch and descending aorta. Type A is characterized by a higher incidence of early complications and high prehospital mortality.
With the flow, dissecting aortic aneurysms can be acute (from several hours to 1-2 days), subacute (from several days to 3-4 weeks) and chronic (several months).
Symptoms of aortic dissecting aneurysm
The clinical picture of the disease is due to the presence and length of aortic dissection, intraparietal hematoma, compression and occlusion of aortic branches, and ischemia of vital organs. There are several options for the development of dissecting aortic aneurysm: the formation of an extensive unbroken hematoma; wall dissection and hematoma breakthrough into the aortic lumen; wall separation and hematoma breakthrough into the surrounding aorta tissue; aortic rupture without dissection of the wall.
A sudden onset is characteristic of dissecting aortic aneurysms, with imitation of symptoms of various cardiovascular, neurological, and urological diseases. Aortic dissection is manifested by a sharp increase in tearing, intolerable pain with a wide area of irradiation (behind the sternum, between the shoulder blades and along the spine, in the epigastric region, lower back) migrating along the course of dissection. There is an increase in blood pressure followed by a decline, asymmetry of the pulse in the upper and lower extremities, excessive sweating, weakness, cyanosis, and anxiety. Most patients with dissecting aortic aneurysms die from the development of complications.
Neurological manifestations of pathology can be ischemic damage to the brain or spinal cord (hemiparesis, paraplegia), peripheral neuropathy, impairment of consciousness (fainting, coma).
Dissecting aneurysm of the ascending aorta may be accompanied by myocardial ischemia, compression of the mediastinal organs (appearance of hoarseness, dysphagia, shortness of breath, Horner’s syndrome, superior vena cava syndrome), the development of acute aortic regurgitation, hemopericardium, cardiac tamponade. The separation of the walls of the descending thoracic and abdominal aorta is expressed by the development of severe renovascular hypertension and acute renal failure, acute ischemia of the digestive system, mesenteric ischemia, acute ischemia of the lower extremities.
Diagnosis of dissecting aortic aneurysm
If a dissecting aortic aneurysm is suspected, an urgent and accurate assessment of the patient’s condition is necessary. The main diagnostic methods that allow visualization of aortic damage are chest X-ray, echoCG (transthoracic and transesophageal), UZDG, MRI and CT of the chest / abdominal aorta, aortography. A chest x-ray reveals signs of spontaneous aortic dissection: aortic and upper mediastinum dilation (90% of cases), deformity of the aortic or mediastinal contour shadow, presence of pleural effusion (more often on the left), reduction or absence of pulsation of the enlarged aorta.
A more informative study of dissecting aortic aneurysm, available in any conditions, is considered to be transthoracic or transesophageal echocardiography, which helps determine the condition of the thoracic aorta, identify detached intima flap, true and false channels, assess the viability of the aortic valve, the incidence of atherosclerotic aortic lesions.
Performing CT and MRI for dissecting aortic aneurysm requires a stable condition of the patient for transportation and the procedure. CT scan is used to detect intramural hematoma, penetration of atherosclerotic ulcers of the thoracic aorta. MRI allows, without the use of intravenous contrast media, to accurately determine the localization of the intima, the direction of dissection in the direction of blood flow in the false channel, to assess the involvement of the main branches of the aorta, the state of the aortic valve.
Aortography is an invasive but highly sensitive method for studying aortic aneurysm; allows you to see the place of the initial strain, localization and length of the bundle, true and false lumens, the presence of proximal and distal fenestration, the degree of viability of the aortic valve and coronary arteries, the integrity of the aortic branches.
It is necessary to carry out differential diagnostics of dissecting aortic aneurysm with acute myocardial infarction, occlusion of mesenteric vessels, renal colic, renal infarction, thromboembolism of the aortic bifurcation, acute aortic insufficiency without aortic dissection, nondissocative aneurysm of the ausculta, and no case of an abdominal stropic abdominal system, or an abdominal strapid abdominal arthroplasty without aortic dissection;
Prognosis and prevention of dissecting aortic aneurysm
In the absence of treatment of dissecting aortic aneurysm, mortality is high, during the first 3 months it can reach 90%. Postoperative survival with stratification type A is 80%, type B – 90%. The long-term prognosis is generally favorable: a ten-year survival rate is 60%.
Prevention of the formation of dissecting aortic aneurysm is to monitor the course of cardiovascular diseases. Prevention of aortic dissection includes observation of a cardiologist, monitoring of blood pressure and blood cholesterol level, intermittent USDG or ultrasound of the aorta.



Hello! I could have sworn I’ve been to this blog before but after browsing through some of the post I realized it’s new to me. Anyways, I’m definitely happy I found it and I’ll be book-marking and checking back frequently!
I really like it when folks come together and share ideas. Great website, keep it up.
I believe that avoiding ready-made foods would be the first step to lose weight. They will often taste fine, but packaged foods include very little vitamins and minerals, making you eat more simply to have enough strength to get through the day. If you are constantly ingesting these foods, moving over to grain and other complex carbohydrates will let you have more strength while taking in less. Great blog post.
Thanks for these guidelines. One thing I should also believe is the fact credit cards providing a 0 monthly interest often appeal to consumers with zero rate of interest, instant approval and easy online balance transfers, nonetheless beware of the number one factor that will void your own 0 easy neighborhood annual percentage rate and also throw you out into the bad house rapidly.
Thanks for the helpful content. It is also my belief that mesothelioma has an incredibly long latency time period, which means that symptoms of the disease might not emerge until finally 30 to 50 years after the primary exposure to mesothelioma. Pleural mesothelioma, that is certainly the most common type and has effects on the area round the lungs, may cause shortness of breath, breasts pains, and also a persistent coughing, which may produce coughing up blood vessels.