Surgical treatment of atherosclerosis is indicated in cases of high threat or development of artery occlusion by a plaque or thrombus.
Both open surgery (endarterectomy) and endovascular surgery are performed on the arteries with dilation of the artery with the help of balloon catheters and installation of a stent at the site of the narrowing of the artery, which prevents vessel blockage.
In patients with severe atherosclerosis of the heart vessels, threatening the development of myocardial infarction, coronary artery bypass surgery is performed.
In the treatment of atherosclerosis adhere to the following principles:
- restriction of cholesterol entering the body and reduction of its synthesis by tissue cells;
- increased excretion of cholesterol and its metabolites from the body;
- use of estrogen replacement therapy in women in menopause;
- exposure to infectious pathogens.
Cholesterol intake is restricted by prescribing a diet that excludes cholesterol-containing foods.
For the medical treatment of atherosclerosis using the following groups of drugs:
- Nicotinic acid and its derivatives – effectively reduce the content of triglycerides and cholesterol in the blood, increase the content of high-density lipoproteins with anti-atherogenic properties. The prescription of nicotinic acid drugs is contraindicated in patients with liver diseases.
- Fibrates (clofibrate) – reduce the synthesis in the body’s own fats. They can also cause disorders in the liver and the development of cholelithiasis.
- Bile acid sequestrants (cholestyramine, colestipol) – bind and remove bile acids from the intestine, thereby lowering the amount of fat and cholesterol in the cells. With their use may be marked constipation and flatulence.
- Preparations of the group of statins (lovastatin, simvastatin, pravastatin) are most effective for lowering cholesterol, since they reduce its production in the body itself. Apply statins at night, because at night the synthesis of cholesterol increases. Can lead to abnormal liver function.
Atherosclerosis is a systemic lesion of arteries of large and medium caliber, accompanied by accumulation of lipids, proliferation of fibrous fibers, dysfunction of the vascular wall endothelium and leading to local and general hemodynamic disorders. Atherosclerosis can be the pathological basis of coronary artery disease, ischemic stroke, obliterating lesions of the lower extremities, chronic occlusion of the mesenteric vessels, etc. The diagnostic algorithm includes determining blood lipids, performing ultrasound of the heart and blood vessels, and angiographic studies. In atherosclerosis, medical therapy, diet therapy, and, if necessary, revascularizing surgical interventions are carried out.
Atherosclerosis is a lesion of the arteries, accompanied by cholesterol deposits in the inner lining of blood vessels, a narrowing of their lumen and a malfunction in the blood supply to the organ. Atherosclerosis of the heart vessels is manifested mainly by attacks of angina pectoris. Leads to the development of coronary heart disease (CHD), myocardial infarction, cardiosclerosis, vascular aneurysm. Atherosclerosis can lead to disability and premature death.
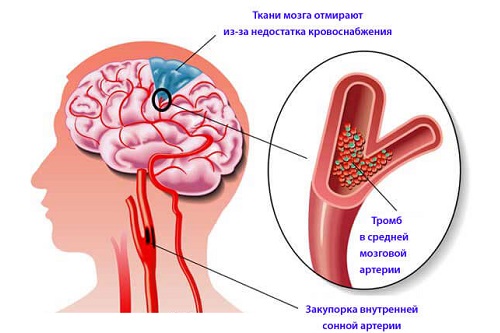
In atherosclerosis, the arteries of medium and large caliber, elastic (large arteries, aorta) and muscular-elastic (mixed: carotid, arteries of the brain and heart) types are affected. Therefore, atherosclerosis is the most common cause of myocardial infarction, ischemic heart disease, cerebral stroke, circulatory disorders of the lower extremities, abdominal aorta, mesenteric and renal arteries.
In recent years, the incidence of atherosclerosis has become rampant, outpacing the causes of injury, infectious and oncological diseases at the risk of developing disability, disability and mortality. Atherosclerosis occurs most frequently in men older than 45-50 years old (3-4 times more often than women), but it occurs in younger patients.
The mechanism of atherosclerosis
In atherosclerosis, a systemic arterial lesion occurs as a result of disturbances in lipid and protein metabolism in the walls of blood vessels. Metabolic disorders are characterized by a change in the ratio between cholesterol, phospholipids and proteins, as well as the excessive formation of β-lipoproteins.
It is believed that in its development atherosclerosis goes through several stages:
- Stage I – lipid (or fat) spot. For the deposition of fat in the vascular wall an essential role is played by microdamages of arterial walls and local blood flow slowing down. The areas of vascular branches are most susceptible to atherosclerosis. The vascular wall loosens and swells. Arterial wall enzymes tend to dissolve lipids and protect its integrity. When protective mechanisms are depleted, complex areas of compounds consisting of lipids (mainly cholesterol) and proteins form in these areas and they are deposited in the intima (inner membrane) of the arteries. The duration of the lipid stain stage is different. Such fatty spots are visible only under a microscope, they can be detected even in infants.
- Stage II – liposclerosis. It is characterized by the growth of young connective tissue in the areas of fat deposits. Gradually, an atherosclerotic (or atheromatous) plaque is formed, consisting of fats and connective tissue fibers. At this stage, atherosclerotic plaques are still liquid and can be dissolved. On the other hand, they are dangerous, since their loose surface may rupture, and fragments of plaques – to clog the lumen of the arteries. The vessel wall at the site of attachment of the atheromatous plaque loses its elasticity, cracks and ulcers, leading to the formation of blood clots, which are also a source of potential danger.
- Stage III – atherocalcinosis. Further formation of plaque is associated with its compaction and deposition of calcium salts in it. Atherosclerotic plaque can behave stably or gradually grow, deforming and narrowing the lumen of the artery, causing a progressive chronic disruption of the blood supply to the organ affected by the artery. At the same time, there is a high probability of acute occlusion ( occlusion ) of the vessel lumen with a thrombus or fragments of a disintegrated atherosclerotic plaque with the development of a site of infarction (necrosis) or gangrene in the blood supply to the artery of the limb or organ.
This point of view on the mechanism of the development of atherosclerosis is not the only one. There are opinions that infectious agents play a role in the development of atherosclerosis (herpes simplex virus, cytomegalovirus, chlamydial infection, etc.), hereditary diseases accompanied by an increase in cholesterol level, mutations of vascular wall cells, etc.
Factors of atherosclerosis
Factors affecting the development of atherosclerosis are divided into three groups: non-removable, disposable, and potentially disposable.
Fatal factors include those that cannot be excluded by volitional or medical influence.
These include:
- Age. With age, the risk of atherosclerosis increases. Atherosclerotic changes in blood vessels are more or less observed in all people after 40-50 years.
- Paul. In men, the development of atherosclerosis occurs ten years earlier and exceeds the incidence of atherosclerosis among women 4 times. After 50-55 years, the incidence of atherosclerosis among women and men is evened out. This is due to a decrease in the production of estrogens and their protective function in women during menopause.
- Burdened family heredity. Often, atherosclerosis develops in patients whose relatives suffer from this disease. It is proved that heredity in atherosclerosis contributes to the early (up to 50 years) development of the disease, while after 50 years genetic factors do not have a leading role in its development.
Eliminate factors of atherosclerosis are those that can be excluded by the person himself by changing the habitual way of life.
These include:
- Smoking. Its effect on the development of atherosclerosis is explained by the negative effects of nicotine and tar on the vessels. Long-term smoking several times increases the risk of hyperlipidemia, hypertension, coronary artery disease.
- Unbalanced nutrition. Eating large amounts of animal fats accelerates the development of atherosclerotic vascular changes.
- Hypodynamia. Maintaining a sedentary lifestyle contributes to the violation of fat metabolism and the development of obesity, diabetes, vascular atherosclerosis.
Potentially and partially removable risk factors include those chronic disorders and diseases that can be corrected by means of prescribed treatment.
These include:
- Arterial hypertension. Against the background of high blood pressure, conditions are created for the increased soaking of the vascular wall with fats, which contributes to the formation of an atherosclerotic plaque. On the other hand, a decrease in the elasticity of arteries in atherosclerosis contributes to the maintenance of elevated blood pressure.
- Dyslipidemia. Disruption of fat metabolism in the body, manifested by a high content of cholesterol, triglycerides and lipoproteins, plays a leading role in the development of atherosclerosis.
- Obesity and diabetes. Increase the likelihood of atherosclerosis by 5-7 times. This is due to a violation of fat metabolism, which is the basis of these diseases and is the trigger mechanism of atherosclerotic vascular lesions.
- Infection and intoxication. Infectious and toxic agents have a damaging effect on the vascular walls, contributing to their atherosclerotic changes.
Knowledge of the factors contributing to the development of atherosclerosis is especially important for its prevention, since the influence of avoidable and potentially avoidable circumstances can be weakened or completely eliminated. Elimination of adverse factors can significantly slow down and facilitate the development of atherosclerosis.
Symptoms of Atherosclerosis
In atherosclerosis, the thoracic and abdominal parts of the aorta, the coronary, mesenteric, renal vessels, as well as the arteries of the lower extremities and the brain are more often affected. In the development of atherosclerosis, there are preclinical (asymptomatic) and clinical periods. In the asymptomatic period, an elevated level of β-lipoproteins or cholesterol is detected in the blood in the absence of symptoms of the disease. Clinically, atherosclerosis begins to manifest itself when the arterial lumen is narrowed by 50% or more. During the clinical period, there are three stages: ischemic, trombonekrotichesky and fibrous.
In the stage of ischemia, insufficient blood supply to an organ develops (for example, myocardial ischemia due to atherosclerosis of the coronary vessels is manifested by angina). Thrombonecrotic stage is accompanied by thrombosis of the altered arteries (for example, the course of coronary atherosclerosis may be complicated by myocardial infarction). At the stage of fibrotic changes, proliferation of connective tissue occurs in poorly supplied organs (for example, atherosclerosis of the coronary arteries leads to the development of atherosclerotic cardiosclerosis).
The clinical symptoms of atherosclerosis depend on the type of affected arteries. A manifestation of atherosclerosis of the coronary vessels are angina, myocardial infarction and cardiosclerosis, consistently reflecting the stages of circulatory failure of the heart.
The course of aortic atherosclerosis is long and asymptomatic for a long time, even in severe forms. Atherosclerosis of the thoracic aorta is clinically manifested by aortalgia – pressing or burning pain behind the sternum, radiating to the arms, back, neck, upper abdomen. Unlike the pain of angina pectoris, aortalgia can last for several hours and days, periodically weakening or increasing. A decrease in the elasticity of the aortic wall causes an increase in the work of the heart, leading to hypertrophy of the left ventricular myocardium.
Atherosclerotic lesion of the abdominal aorta is manifested by abdominal pain of different localization, flatulence, and constipation. At atherosclerosis of the bifurcation of the abdominal aorta, numbness and coldness of the legs, edema and hyperemia of the feet, necrosis and ulcers of the toes, intermittent claudication are observed.
Manifestations of atherosclerosis of the mesenteric arteries are attacks of the “abdominal toad” and impaired digestive function due to insufficient blood supply to the intestine. Patients experience sharp pains a few hours after eating. Pain localized in the navel or upper abdomen. The duration of a painful attack is from several minutes to 1-3 hours, sometimes the pain syndrome is stopped by taking nitroglycerin. There are bloating, belching, constipation, palpitations, increased blood pressure. Later, fetid diarrhea with fragments of undigested food and undigested fat join.
Atherosclerosis of the renal arteries leads to the development of renovascular symptomatic hypertension. Erythrocytes, protein, cylinders are determined in urine. With unilateral atherosclerotic lesion of the arteries, there is a slow progression of hypertension, accompanied by persistent changes in the urine and steadily high numbers of blood pressure. Bilateral lesion of the renal arteries causes malignant arterial hypertension.
At atherosclerosis of cerebral vessels there is a decrease in memory, mental and physical performance, attention, intelligence, dizziness, and sleep disorders. In cases of marked atherosclerosis of the brain, the behavior and psyche of the patient changes. Atherosclerosis of the arteries of the brain may be complicated by an acute violation of cerebral circulation, thrombosis, hemorrhage.
Manifestations of atherosclerosis obliterans of lower limb arteries are weakness and pain in the calf muscles of the leg, numbness and chilliness of the legs. Characteristic development of the syndrome of “intermittent claudication” (pain in the calf muscles occur when walking and subside at rest). Cooling, paleness of the limbs, trophic disorders (desquamation and dryness of the skin, development of trophic ulcers and dry gangrene) are noted.
Complications of Atherosclerosis
Complications of atherosclerosis are chronic or acute vascular insufficiency of the blood supplying organ. The development of chronic vascular insufficiency is associated with the gradual narrowing (stenosis) of the arterial lumen by atherosclerotic changes – stenotic atherosclerosis.
Chronic insufficiency of blood supply to the organ or its part leads to ischemia, hypoxia, dystrophic and atrophic changes, proliferation of connective tissue and the development of small-sclerosis.
Acute vascular insufficiency is caused by an acute vascular occlusion with a thrombus or embolus, which is manifested by the clinic of acute ischemia and myocardial infarction. In some cases, rupture of the artery aneurysm may be fatal.
Diagnosis of atherosclerosis
Initial data for atherosclerosis is established by ascertaining patient complaints and risk factors. Recommended consultation cardiologist. At the general examination, signs of atherosclerotic lesion of the vessels of internal organs are detected: edema, trophic disorders, weight loss, multiple adipose tissue on the body, etc. Auscultation of heart vessels, aorta reveals systolic noise. For atherosclerosis indicate a change in pulsation of the arteries, increased blood pressure, etc.
Laboratory findings indicate elevated levels of blood cholesterol, low-density lipoprotein, triglycerides. X-ray on aortography reveals signs of aortic atherosclerosis: its lengthening, compaction, calcification, expansion in the abdominal or thoracic regions, the presence of aneurysms. The condition of the coronary arteries is determined by coronary angiography.
Violations of the blood flow in other arteries is determined by angiography – contrast x-ray of blood vessels. At atherosclerosis of the arteries of the lower extremities, according to the angiography, their obliteration is recorded. With the help of USDG of renal vessels, atherosclerosis of the renal arteries and the corresponding renal dysfunction are detected.
Methods of ultrasound diagnosis of the arteries of the heart, lower limbs, aorta, carotid arteries register a decrease in the main blood flow through them, the presence of atheromatous plaques and blood clots in the lumen of blood vessels. Reduced blood flow can be diagnosed using lower limb reovasography.
Forecast and prevention of atherosclerosis
In many ways, the prognosis of atherosclerosis is determined by the behavior and lifestyle of the patient himself. Elimination of possible risk factors and active drug therapy can delay the development of atherosclerosis and achieve improvement in the patient’s condition. With the development of acute circulatory disorders with the formation of foci of necrosis in the organs, the prognosis worsens.
In order to prevent atherosclerosis, smoking cessation, elimination of the stress factor, switching to low-fat and cholesterol-poor food, systematic physical activity commensurate with the possibilities and age, and normalization of weight are necessary.
It is advisable to include in the diet of foods containing fiber, vegetable fats (flaxseed and olive oils), which dissolve cholesterol deposits. The progression of atherosclerosis can be slowed down by taking cholesterol-lowering drugs.


hi!,I love your writing very much! percentage we keep in touch more about your post on AOL? I need an expert in this area to resolve my problem. Maybe that’s you! Looking ahead to look you.
Hello, I enjoy reading through your article post.
I wanted to write a little comment to support you.