Nosocomial infections – a variety of infectious diseases, infection which occurred in a medical establishment.
Depending on the degree of diffusion distinguish between generalized (bacteremia, septicemia, pyosepticemia, bacterial shock) and localized forms of nosocomial infections (lesions of the skin and subcutaneous tissue, respiratory, cardiovascular, urogenital system, bones and joints, CNS etc.).
Identification of pathogens of nosocomial infections is carried out using methods of laboratory diagnostics (microscopic, microbiological, serological, molecular-biological). In the treatment of nosocomial infections the use of antibiotics, antiseptics, adjuvants, physical therapy, blood purification etc.
Nosocomial infection
Nosocomial (hospital, nosocomial) infections, infectious diseases of different etiologies that have occurred to the patient or medical officer in connection with stay in medical institution. An infection is considered nosocomial if it developed no sooner than 48 hours after admission the patient to the hospital.
The prevalence of nosocomial infections (NI) in medical institutions of different profile is 5-12%. The largest share of hospital-acquired infections on obstetric and surgical departments (departments of intensive care, abdominal surgery, trauma, burn injury, urology, gynecology, otolaryngology, dentistry, Oncology, etc.). Nosocomial infections are of great medical and social problem because weight for underlying disease, increase the duration of treatment in 1.5 times, and the number of deaths – 5 times.
Etiology and epidemiology of nosocomial infections
The main causative agents of nosocomial infections (85% of the total) are opportunistic pathogens: gram-positive cocci (epidermidis and Staphylococcus aureus, beta-hemolytic Streptococcus, pneumococcus, Enterococcus) and gram-negative rod-shaped bacteria (Klebsiella, Escherichia, Enterobacter, Proteus, Pseudomonas, etc.).
In addition, in the etiology of nosocomial infections a large proportion of the role of viral pathogens herpes simplex, adenovirus infection, influenza, parainfluenza, cytomegalovirus, viral hepatitis, respiratory syncytial infections, and rhinoviruses, rotaviruses, enteroviruses, and so nosocomial infection can be caused by opportunistic and pathogenic fungi (yeasts, molds, radiant). Feature of hospital-acquired strains of conditionally pathogenic microorganisms is their high variability, drug resistance, and resistance to environmental factors (ultraviolet radiation, disinfectants, etc.).

Sources of nosocomial infections in most cases are the patients or the medical staff who are carriers or diseased erased and manifest forms of pathology. Studies show that the role of third parties (in particular, visitors of hospitals) in the spread of nosocomial infection is low. Transmission of various forms of hospital infections is implemented through airborne droplets, fecal-oral, contact, vector-borne mechanism. In addition, possible parenteral route of transmission of nosocomial infection during various invasive medical procedures: blood collection, injections, vaccination, instrumental manipulations, surgeries, mechanical ventilation, hemodialysis, etc. So the hospital may be infected with hepatitis b, C and D, purulent-inflammatory diseases, syphilis, and HIV infection. Known cases of nosocomial outbreaks of Legionnaires ‘ disease in the patients receiving the therapeutic shower and whirlpool baths.
Factors involved in the spread of nosocomial infection, there may be contaminated care items and furnishings, medical instruments and apparatus, solutions for infusion therapy, clothing and hands of medical staff, medical products reusable (probes, catheters, endoscopes), drinking water, bedding, suture and dressings, and more..
The importance of certain types of nosocomial infections depends largely on the profile of the medical institution. So, in burn units dominated by Pseudomonas infection that is mainly transmitted through the objects of care and hands of staff as the main source of nosocomial infection are the patients themselves. In maternity services, the main problem is a staph infection, disseminated health personnel carrier of Staphylococcus aureus.
Urology departments dominates the infection caused by gram-negative flora: Escherichia, Pseudomonas aeruginosa, and others In the pediatric hospitals of special importance was the problem of the spread of childhood infections – chickenpox, mumps, rubella, measles. The emergence and spread of hospital-acquired infections contribute to the violation of sanitary-epidemiological regime of the hospitals (lack of personal hygiene, asepsis and antisepsis, modes of disinfection and sterilization, delayed detection and isolation of individuals-sources of infection, etc.).
To the risk group most likely to develop nosocomial infection are neonates (especially premature) and infants; elderly and debilitated patients, persons suffering from chronic diseases (diabetes, blood diseases, renal failure), immune deficiencies, cancer. Sensitivity to nosocomial infection increases if you have open wounds, abdominal drains, intravascular and urinary catheters, tracheostomy and other invasive devices. The occurrence and severity of hospital-acquired infections is affected by a long stay in hospital, long-term antibiotic therapy, immunosuppressive therapy.
Classification of nosocomial infections
For the duration of the course of nosocomial infections are divided into acute, subacute and chronic; according to the severity of the clinical manifestations – for light, moderate and severe forms. Depending on the extent of the infectious process distinguish between generalized and localized forms of nosocomial infection. Generalized infection presents with bacteremia, septicemia, bacterial shock.

In turn, among the localized forms of release:
- infections of the skin, mucous membranes and subcutaneous tissue, including post-operative, burns, traumatic wounds. In particular, these include omphalitis, abscesses and cellulitis, pyoderma, erysipelas, mastitis, abscess, fungal skin infections etc.
- infection of the mouth (stomatitis) and ENT-organs (tonsillitis, pharyngitis, laryngitis, epiglottitis, rhinitis, sinusitis, otitis, mastoiditis)
- infection of the bronchopulmonary system (bronchitis, pneumonia, pleurisy, lung abscess, gangrene of the lung, empyema, mediastinitis)
- infection of the digestive system (gastritis, enteritis, colitis, viral hepatitis)
- eye infection (blepharitis, conjunctivitis, keratitis)
- infection of the urogenital tract (bacteriuria, urethritis, cystitis, pyelonephritis, endometritis, adnexitis)
- infections of bones and joints (bursitis, arthritis, osteomyelitis)
- infection of the heart and blood vessels (pericarditis, myocarditis, endocarditis, phlebitis, thrombophlebitis).
- CNS infection (brain abscess, meningitis, myelitis, etc.).
In the structure of nosocomial infections on a share of purulent-septic diseases account for 75-80%, intestinal infections – 8-12%, blood-contact infection – 6-7%. Other infectious diseases (rotavirus, diphtheria, tuberculosis, mycosis, etc.) accounts for about 5-6%.
Diagnosis of nosocomial infections
The criteria for thinking about the development of nosocomial infections are: the appearance of clinical symptoms not earlier than 48 hours after admission to the hospital; connection with carrying out invasive interventions; establishing the source of infection and factors of transmission. Final judgment on the nature of the infectious process was obtained after the identification of the strain of the pathogen by laboratory diagnostics.
To exclude or confirm bacteremia is the bacterial inoculation of blood on sterility, preferably at least 2-3 times. In localized forms of nosocomial infections microbiological isolation of the pathogen can be produced from other biological media, in connection with which is performed a urine culture, stool, sputum, discharge of wounds, material from a throat, a smear of the conjunctiva, the genital tract the microflora of the. In addition to the culture method of identification of causative agents of nosocomial infections are used in microscopy, serological reactions (RSK, RA, ELISA, RIA), virological, molecular biological (PCR) methods.
Treatment of nosocomial infections
The complexity of the treatment of nosocomial infections due to its development in a weakened body, on the background of the underlying pathology and drug resistance of hospital strains to traditional pharmacotherapy. Patients with diagnosed infectious processes must be isolated; the Department carried out careful current and final disinfection. The choice of antimicrobial drug is based on the characteristics antibiogram: in nosocomial infections caused by gram-positive flora the most effective vancomycin; gram-negative organisms is carbapenems, cephalosporins of IV generation, aminoglycosides. Perhaps the additional use of specific bacteriophages, Immunostimulants, interferon leukocyte mass, vitamin therapy.
If necessary, conducted transcutaneous irradiation of blood (vlok, UFOC), extracorporeal (hemosorption, limfosorbtsiya). Symptomatic therapy is carried out taking into account the clinical forms of nosocomial infections with participation of specialists: surgeons, traumatologists, dermatologists, otolaryngologists, pulmonologists, ophthalmologists, urologists, gynecologists, cardiologists, neurologists, etc.
Prevention of nosocomial infections
The main measures of prevention of nosocomial infections are reduced to comply with sanitary-hygienic and anti-epidemic requirements. First of all, it concerns the mode of disinfection of premises and objects of care, application of modern highly effective antiseptics, the quality of pre-sterilization processing and sterilization of instrumentation, unobjectionable following the rules of asepsis and antisepsis.
The medical staff must comply with the measures of individual protection when carrying out invasive procedures: wear rubber gloves, goggles and mask; careful medical instrumentation. Of great importance in the prevention of nosocomial infections is vaccination of healthcare workers against hepatitis b, rubella, influenza, diphtheria, tetanus, and other infections. All employees of the MPI are regularly scheduled follow-up inspection aimed at detection of carriers of pathogens. To prevent the occurrence and spread of nosocomial infections will allow reducing the time of patient hospitalization, rational antibiotic therapy, the validity of invasive diagnostic and therapeutic procedures, and epidemiological control in hospitals.


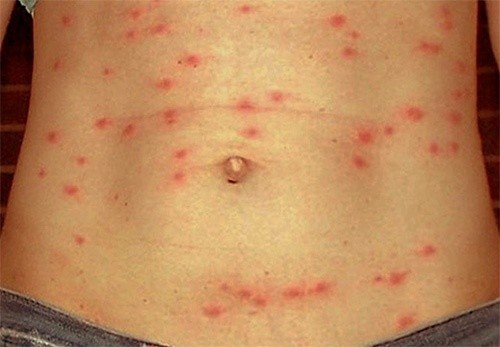

Hello!
Love the septic content on your site! You know, most websites get traffic from their blogs, and we feel that you could use a little boost, since you are not blogging daily yet.
Writing takes a lot of time, and we have just the team to come up with great content you are looking for.
You can have a brand new article to post on osvilt.com starting at $10 in as little as 5 days!
Hi!
Love the septic content on your site! You know, websites get traffic from their blog, and we feel that you could use a little boost, since you are not blogging weekly yet.
Blogging takes a lot of time and effort, and we have just the team from US/Canada to come up with great content you are looking for.
You can have your new article to post on your website starting at $10 in as little as 5 business days!
Depending on the extent of the infectious process distinguish between generalized and localized forms of nosocomial infection. Generalized infection presents with bacteremia, septicemia, bacterial shock.
infections of the skin, mucous membranes and subcutaneous tissue, including post-operative, burns, traumatic wounds. In particular, these include omphalitis, abscesses and cellulitis, pyoderma, erysipelas, mastitis, abscess, fungal skin infections etc.
Definitely consider that that you said. Your favorite reason appearedto be at the web the easiest thing to consider of.I say to you, I definitely get irked at the same time as otherpeople consider issues that they plainly don’t knowabout. You controlled to hit the nail upon the highest as well as outlinedout the entire thing without having side effect , people could take asignal. Will probably be again to get more. Thank you
I could agree more- and maybe I should!! jk
Sensitivity to nosocomial infection increases if you have open wounds, abdominal drains, intravascular and urinary catheters, tracheostomy and other invasive devices.
Urology departments dominates the infection caused by gram-negative flora: Escherichia, Pseudomonas aeruginosa, and others In the pediatric hospitals of special importance was the problem of the spread of childhood infections – chickenpox, mumps, rubella, measles.
Juventus forward Amauri has turned down moves to Fulham and West Brom, his agent today claimed. The Italy international has yet to score a Serie A goal in the current campaign. Amauri too good for Fulham and West Brom, claims Juve striker’s agent
With havin so much content do you ever run into any issues of plagorism or copyright infringement? My blog has a lot of exclusive content I’ve either authored myself or outsourced but it appears a lot of it is popping it up all over the internet without my authorization. Do you know any methods to help protect against content from being stolen? I’d really appreciate it.
Wow, marvelous weblog layout! How lengthy have you been blogging for? you made blogging glance easy. The overall look of your website is fantastic, as well as the content!
Hi, Neat post. There is an issue with your website in web explorer, would test this¡K IE still is the market chief and a huge element of folks will pass over your great writing due to this problem.
my file cabinets are made of recycled fiber, they are great for holding large file folders~