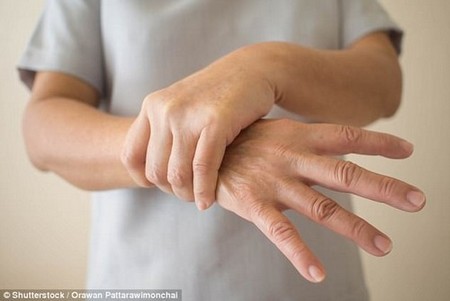
Recently, I went for an MRI scan and was told I have a slipped disc pressing on a nerve, which is causing pain down my left leg. I was prescribed 300mg gabapentin, to be taken three times a day for a week, which had to increase to 600mg a day for the second week.
I am still in pain and worried that this is the wrong approach. Surely the slipped disc is the problem, and something should be done to alleviate that?
In answering your question, let me first explain something about what has happened to you and how your condition is likely to progress.
A slipped or herniated disc occurs when one of the rubbery discs that lie between the bony vertebrae in the back and act as shock absorbers ruptures.
Each disc comprises a tough outer fibrous ring enclosing a softer centre. If the disc degenerates with age, or trauma, then the soft interior can bulge out through a breach in the outer ring and press on one or more nerves in the spinal cord – the bundle of nerves that extends from the brain down to the level of your lowest ribs.
If a nerve is impinged upon, there may be referred pain, which is pain felt not at the site of the damaged disc, but instead in the region that the nerve supplies, such as the legs or buttocks.
The pain you have is called sciatica, as it is the sciatic nerve, which exits the lower part of the spine, one branch to the left leg, the other to the right, that is impinged upon in this case.
The object of treatment is to reduce pain but, as you point out, it does not address the underlying cause.
Sadly, the anatomy is not so simple that we can push the herniated disc back into place. Instead, symptoms typically improve in time when the disc material shrinks back and the prolapsed disc heals – this can take days or months.
Painkillers ranging from paracetamol to non-steroidal anti-inflammatory drugs (NSAIDs) are the mainstay of treatment.
It also helps to restrict, as much as is practical, any activity that might worsen the pain – this differs from individual to individual.
Some patients find that sitting or reclining provides relief from symptoms; others find the pain is worse even when resting in bed.
Losing weight if you are overweight is beneficial, as it reduces the pressure on the lower back.
Gabapentin is helpful in some patients with nerve-derived pain, and the current thinking is that this buys you some relief while you wait for the disc to heal.
The object of treatment is to reduce pain but, as you point out, it does not address the underlying cause
I assume that the decision to prescribe gabapentin was because you did not obtain relief from simple painkillers or NSAIDs.
If your symptoms do not resolve as the weeks and months pass, or if the pain becomes more severe or there is weakness in the leg, then surgery may be considered.
This involves partial or complete removal of the herniated disc, and is carried out under general anaesthetic by a spinal surgeon or a neurosurgeon.
If your symptoms don’t improve, I would ask your GP for a referral to a spinal surgeon.
But rest assured that while your current treatment may sound conservative, it is highly likely to be effective.
Around 18 months ago, I started to sweat when doing anything: shopping, gardening, even climbing stairs. My periods have also been irregular.
My GP said it was likely that I am menopausal (I am 49) and my sweats were probably bad as I was fat. I am 21 st and 5 ft 8 in.
Another GP suggested thinking about hormone replacement therapy (HRT) but, because of my weight, said this could be a problem. I am now exploring the herbal route: I’m on black cohosh, which so far is having no effect.
As more than 90 per cent of women become menopausal between the ages of 45 and 55, I suspect that this is the most likely cause of your sweating.
During the perimenopause, the run-up to the menopause (which occurs a year after the last period), levels of oestrogen fall and this causes the temperature regulation area of the hypothalamus, a region of the brain just above the pituitary gland at the base of the brain, to behave abnormally.
Under normal circumstances, the hypothalamus will initiate mechanisms to cool the body when its temperature increases by more than 0.4c. Blood flow to the skin then increases, causing flushing and a rise in sweat production.
However, in menopausal women, when oestrogen falls below a certain level, those heat loss mechanisms are triggered at much lower changes in temperature, possibly due to some change in the cells of the hypothalamus.
That is why you are sweating with minimal physical activity – the control mechanism in your brain has become oversensitive.
Your weight does put you at increased risk.
Obese postmenopausal women have higher oestrogen levels than thinner women, as a hormone also produced by the ovaries, called androstenedione, is converted in body fat to oestrone, a form of oestrogen, yet, for ill-understood reasons, this paradoxically makes hot flushes and sweats far more likely. Your doctor may have reservations about prescribing hormone replacement therapy (HRT) – which contains oestrogen – but it will be effective. The oestrogen seems to reset the behaviour of the hypothalamus.
I would counsel against herbal remedies, as there is a lack of research to confirm either their effectiveness or safety.
The most effective and proven alternatives to HRT are some of the selective serotonin reuptake inhibitor (SSRI) antidepressant drugs. Venlafaxine, paroxetine, and citalopram have all been found to relieve menopausal symptoms in some patients, but, as with HRT, a balance has to be struck between the benefits and potential side-effects, which include drowsiness, nausea, a loss of appetite and interference with sexual function.
The one action you can take to cut your sweats is to reduce your body mass index (BMI) to below 30. At 5 ft 8 in, you should ideally weigh around 11 st.
At your current weight, you are a candidate for bariatric (weight loss) surgery. However, with the help of a dietitian, in tandem with your strong motivation, achieving a lower BMI is possible without resorting to surgery, and will help reduce the symptoms that trouble you.
IN MY VIEW… YOU GET SECOND-CLASS CARE ONLINE
By the start of this year, there were at least 34 online GP service providers registered in Britain.
Yet the inspector established to ensure that these ‘virtual doctors’ provide effective medical care has found 43 per cent of them do not meet patient safety criteria.
The concerns included inappropriate prescribing of antibiotics and failure to collect patient information from their GPs.
But, for me, the real issue with this kind of online doctoring is the potential for misdiagnosis. In my practice, we ensured there were doctors available on the phone for those unable to visit the surgery. Our patients were also able to email us.
Although this was all popular with the patients, we found that it mostly resulted in us asking them to attend for a physical examination, in order to make a diagnosis correctly. As doctors, we felt the information given over the phone just wasn’t enough.
To make a correct diagnosis requires taking a careful history and a physical examination, often supplemented by some tests.
These new online doctors abandon the idea of any physical contact with the patient.
That is why you are sweating with minimal physical activity – the control mechanism in your brain has become oversensitive
The consultation is typically by telephone, video or email – but seeing a small picture of a person talking at the top of your mobile phone is no substitute for a face-to-face discussion and a physical examination.
What if the patient has earache? How can an online or telephone consultation distinguish between otitis media (a middle ear infection) and otitis externa (infection of the lining of the ear canal)?
And what about a patient phoning the doctor for help with a severe sore throat? How can a doctor tell if the patient has acute tonsillitis or glandular fever?
And how can a decision be made whether antibiotics are necessary?
The list of possible pitfalls is endless and there is the constant hazard of missing more sinister and worrying disorders.
I have strong reservations and believe that we are being led by commercial interests into second-class care. Only time will tell, but I hope the inspectors will continue to keep a close eye on such online services.