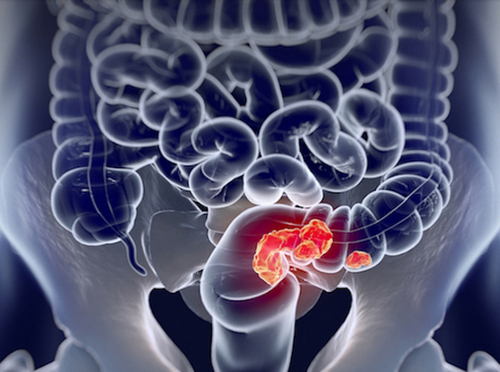
Wounded from battle, ancient Egyptian soldiers would fill their injuries with copper filings that would come off their swords as they sharpened them.
The idea was that this would prevent the wounds getting infected and speed up healing – though they didn’t quite understand how it worked at the time.
Now, 5,000 years later, researchers have resurrected this idea as a way to treat infections and counter the devastating rise of bacterial resistance that’s rendering many of our antibiotics useless.
Research has shown that copper has a powerful antibacterial effect, shutting down energy production in the bacteria and damaging their DNA. Not only does this kill the bugs, but damaging DNA also means the bacteria cannot develop resistance to copper.
A 2015 study of three intensive care units in the U.S. showed introducing copper fittings slashed infection rates by nearly 60 per cent, reported the Health Environments Research & Design Journal. Now, copper-based door handles, bed rails and chairs are being trialled in hospitals in the UK to reduce infections.
This is just one of the methods that researchers in the UK are investigating as a way to kill bacteria and counter the impact of antibiotic resistance.

Researchers in the UK are investigating a way to kill bacteria and counter antibiotic resistance. Men’s beards could harbour future antibiotics – a team have found that certain bacteria grown from beard samples could kill a form of drug-resistant E.coli
Around 25,000 people across Europe die every year from bacterial infections, such as pneumonia or sepsis, which no longer respond to antibiotics.
That number is expected to rise significantly, with one projection suggesting that antimicrobial resistance could account for up to ten million deaths a year worldwide by 2050.
England’s Chief Medical Officer Dame Sally Davies has warned we are facing a ‘post-antibiotic apocalypse’, in which something as simple as a urinary tract infection becomes untreatable, while routine procedures such as hip operations would be deadly because of the risk of incurable infection.
Earlier this month, Dame Sally wrote to thousands of gps, warning them they were contributing to the rise of antibiotic-resistant bugs by over-prescribing the drugs.
‘Many harmful bacteria can reproduce in just 20 minutes,’ says Dr Adam Roberts, a senior lecturer in antimicrobial chemotherapy and resistance at the Liverpool School of Tropical Medicine.
‘They go from two to four to eight to millions overnight and, when this happens in a patient, it is catastrophic. They also mutate as they divide and some of these mutations make the bacteria resistant to an antibiotic.’
Bacteria also swap little bits of their genetic code between themselves, known as plasmids. If resistance to an antibiotic arises on a plasmid inside one bug, it can be copied into all the neighbouring bacteria very quickly, making all of them resistant.
One example is mcr-1, which causes resistance to the antibiotic colistin – one of the current last-line antibiotics available for treating infections that don’t respond to any other drugs.
Researchers have already seen this plasmid being transferred from harmful bacteria such as E.coli, which can lead to food poisoning, to bugs that were previously sensitive to colistin – raising serious concerns that it could spread rapidly, making most infections resistant to one of our last options for an effective antibiotic.
Research has shown that copper has a powerful antibacterial effect, shutting down energy production in the bacteria and damaging their DNA. Not only does this kill the bugs, but damaging DNA also means the bacteria cannot develop resistance to copper
‘We’re reaching an antibiotic Armageddon,’ says Derek Butler, of the charity MRSA Action UK, who lost his stepfather and uncle to drug-resistant infections after they were admitted to hospital for unrelated conditions.
With that in mind, researchers have been exploring new ways to tackle antibiotic resistance. While some are making treatments more tailored to avoid unnecessary use of antibiotics, others are developing entirely new drugs. Here, we look at some of the newest – and most ingenious – breakthroughs.
NEW DRUGS FROM BEARD BUGS
It’s impossible to avoid infections completely in a world teeming with bacteria. Ironically, almost all of the antibiotics we have today originally came from other bacteria and fungi – the most famous example is penicillin, made by a type of mould.
It was previously thought bacteria produced antibiotic chemicals to kill off any competitors around them, but researchers increasingly believe some of these molecules are used as chemical ‘messages’ between neighbouring bugs. Once purified and produced in bulk, they turn from humble communicators to potent antibiotics.
‘Many people are looking for new drugs using moulds and bacteria,’ says Dr Roberts. ‘Researchers are looking in all kinds of environments for strange and unusual microbes that could be producing new antibiotics: the bottom of the sea, the mouldy food in your fridge, or the soil in your back garden.’
Other potential sources of new antibiotics include the bacteria on Brazilian leafcutter ants, which normally protect the insects from infections, and the blood of deadly Komodo dragons, which are immune to the harmful bacteria that live in their mouths and cause fatal blood poisoning in their prey.
Even men’s beards could harbour future antibiotics – Dr Roberts and his team have found that certain bacteria grown from beard samples could kill a form of drug-resistant E.coli.
Many bacteria in the environment are notoriously difficult to grow and study in the laboratory, making it tricky to purify enough antibiotics for testing. But new technologies are helping.
One approach is the iChip – a credit card-sized plastic chip full of tiny chambers, each containing a single bacterial cell taken from the soil. The chip is then buried back in the earth, so the bugs can grow; they’re then tested to see whether any are producing interesting, antibiotic-like chemicals.
In 2016, a team from Northeastern University in Boston, in the U.S., used the iChip to discover teixobactin, produced by a previously unknown species of bacteria.
Active against MRSA, a superbug that’s resistant to several widely-used antibiotics, and tuberculosis, teixobactin is the first new antibiotic to be found in 30 years (it’s yet to be tested in trials).
Dr Roberts said: ‘Researchers are looking in all kinds of environments for strange and unusual microbes that could be producing new antibiotics: the bottom of the sea, the mouldy food in your fridge, or the soil in your back garden’
ANTIBIOTICS THAT SCIENCE FORGOT
As well as discovering new antibiotics, researchers are rediscovering old ones.
Dr Alex O’Neill, a group leader at the Antimicrobial Research Centre at the University of Leeds, has been going back through the scientific archives in search of old antibiotics that were never sold or widely used and are now forgotten.
‘There are around 3,000 antibiotics that were discovered in the ‘golden age’ around the 1940s, but most were just left on the shelf,’ he says.
‘In some cases, there are reasons why they’re no good – maybe because of their side-effects – but in many instances, we simply don’t have the information to make the judgment, so we’re re-examining all of their biological properties.’
The first ‘old’ chemical under the microscope is gamma-actinorhodin, a chemical produced by Streptomyces bacteria. It had been sidelined in favour of more promising drugs. But, working with the Medical Research Council, Dr O’Neill used new techniques to show it was powerful enough to kill even the most dangerous drug-resistant superbugs.
Another idea comes from Dr Andrew Truman at the John Innes Centre in Norwich, who has been focusing on bicyclomycin, a weak antibiotic that was briefly used to treat traveller’s diarrhoea in the Sixties. Despite being relatively ineffective on its own, the latest research suggests bicyclomycin becomes lethal in combination with other commonly used antibiotics.
Unlike many of today’s drugs, which work by messing up the cellular processes inside bacteria so they can no longer multiply, bicyclomycin breaks bacteria’s DNA into pieces – this quickly kills them completely, rather than just stopping them from multiplying.
‘Dead bacteria can’t develop resistance,’ says Dr Truman. ‘If you leave any alive, then resistance can develop.’
USING VIRUSES TO BEAT BACTERIA
One of the most intriguing approaches for tackling superbugs is treating them with viruses known as bacteriophages that have the ability to get inside bacteria.
The viruses then multiply and eventually burst out in search of new bacteria in which to grow, killing the bug in the process.
First discovered in the early 20th century by the English scientist Frederick Twort, bacteriophage therapy became increasingly popular in France, Eastern Europe and Russia.
Professor Martha Clokie, an infectious diseases expert at the University of Leicester, is developing ways to deliver bacteriophages into the gut to treat infections that cause severe diarrhoea, such as C.difficile.
‘A phage that kills one type of bacteria won’t infect another, so you really need to know exactly which bacteria are causing the infection,’ she says.
One of the most intriguing approaches for tackling superbugs is treating them with viruses known as bacteriophages that have the ability to get inside bacteria
‘When people realised how specific phages were, antibiotics seemed a lot better. But, actually, that specificity is what we’re interested in, because it means you can take out a pathogen without harming all the ‘good’ bacteria in the gut.’ There’s a lot of interest in the potential for bacteriophages to treat a wide range of diseases, including infections caused by drug-resistant superbugs.
One team in the Netherlands is about to start a trial of phage therapy for lung infections in people with cystic fibrosis.
Another study is investigating whether bacteriophages can control deep tissue infections in patients with burns.
Unfortunately, bacteria can evolve resistance to bacteriophages in the same way they develop antibiotic resistance. But there are ways around this.
‘Each bacterial species has many different types of phages that can kill it, so if you use a cocktail of many viruses, the bacteria can’t evolve resistance to all of them at once,’ says Professor Clokie.
‘We can also exploit the fact that viruses evolve, too, and ‘train’ our phages by mixing them with resistant bacteria and waiting for them to work out how to kill the bugs again.’
HOW A FAMILY TREE CAN HELP
Thanks to global travel and trade, it’s easier than ever for antibiotic-resistant infections to quickly spread. By teaming up with doctors and scientists across the globe, Dr David Aanensen, director of the Centre for Genomic Pathogen Surveillance at the Wellcome Trust Sanger Institute in Cambridge, is spotting emerging drug-resistant infections sooner, so that public health organisations can take action to contain or limit potential outbreaks before they become major problems.
The team is collecting and analysing DNA in bacterial samples collected from locations around the world, drawing up a ‘family tree’, revealing where the microbes might originally have come from and whether they carry genes that give them resistance to specific antibiotics. The hope is that they can track the emergence of drug-resistant infections, providing up-to-date information to help healthcare organisations.
THE RIGHT DRUG FOR YOUR ILLNESS
Of course, antibiotics remain a crucial treatment for many infections and can save lives. The problem is knowing which one to use.
Currently, doctors send samples to a lab to identify the bacteria responsible for an infection and choose the best drug accordingly.
It can take a day or so to identify the bacteria and weeks or months to get detailed information about which antibiotics will work, due to the slow process of growing and testing bacteria from patient samples.
In the meantime, doctors tend to prescribe patients their ‘best guess’ antibiotic. But there’s no guarantee this will work and the wrong choice could raise the risk of resistant superbugs evolving.
However, now the company Accelerate Diagnostics has invented a machine that can analyse the bacteria in a small sample of blood, cutting the time needed to identify the specific bugs responsible for sepsis, a life-threatening reaction to an infection, to just 90 minutes, compared with days with conventional laboratory testing. It also provides a list of antibiotics that are likely to work within seven hours.
‘The key is getting the right drugs to the right patients at the right dose and at the right time,’ says Daniel Berman, of the innovation foundation NESTA, which is leading a project into new diagnostic tests to reduce antimicrobial resistance.
‘We want to see something similar to a pregnancy test, which could be done at home or a local healthcare setting with an immediate readout.’
Another innovation comes from a research team in India, which has developed a baby’s dummy that changes colour if the child has bacterial blood poisoning.
One disease where a quick diagnostic test would be particularly useful is tuberculosis (TB). Around 250,000 of the deaths worldwide are due to drug-resistant superbugs.
Current tests for antibiotic-resistant bacteria take around two months, because the bacteria responsible for TB grow slowly in the laboratory.
But researchers at the University of Oxford are working on a handheld scanner that analyses the drug-resistant genes in bacteria from a sample of phlegm, providing an answer on the best treatment to use within 24 hours. The device is on trial in Madagascar, Vietnam and India.
‘If you can find out as quickly as possible which drugs are going to work when someone comes into the hospital or clinic, you can get them on the right treatment straight away,’ says Dr Zamin Iqbal, who’s leading the research.
‘You don’t waste time treating them with drugs that don’t work – and you don’t give the bugs a chance to develop resistance.’