Treatment of arterial hypotension begin only after establishing the exact cause of lowering blood pressure. In case of secondary symptomatic hypotension, the main disease will serve as the object of influence.
Neurovegetative genesis hypotension, first of all, requires the correction of vegetative imbalance using drug and non-drug methods.
The complex of medical and recreational activities may include the normalization of the day regimen and nutrition, various options for psychotherapy; neck and collar massage, aromatherapy massage; hydrotherapy (Scottish shower, circular shower, Vichy shower, hydromassage, aromatic and mineral baths); acupuncture, physiotherapy (electrophoresis on the collar area, electrosleep); aromatherapy, aeroionotherapy, exercise therapy.
Drug treatment of arterial hypotension is carried out with drugs of different groups: herbal adaptogens (infusions of lemongrass, aralia, ginseng); anticholinergics, cerebroprotective agents (cinnarizine, vinpocetine); nootropic drugs (glycine, piracetam); antioxidants and vitamins (succinic acid, vitamins A, B, E); antidepressants and tranquilizers. In case of acute arterial hypotension, cardiotonics and vasoconstrictors (mezaton, dopamine), glucocorticoids are administered, and glucocorticoids are administered, and saline and colloid solutions are infused in order to rapidly increase and stabilize blood pressure.
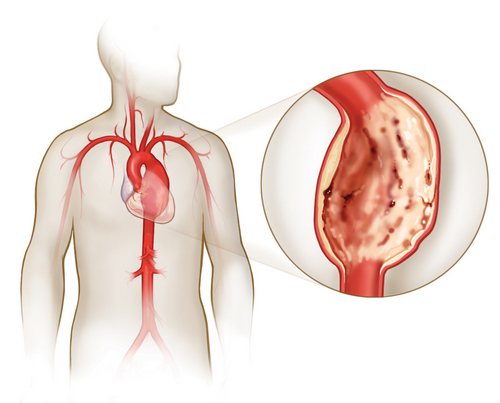
Hypotension (arterial hypotension) is a low blood pressure syndrome characterized by persistent indicators of systolic (upper) pressure of less than 100 mm Hg, and diastolic (lower) of less than 60 mm Hg. Young women and adolescents are more likely to suffer from hypotension. At an older age, on the background of vascular atherosclerosis, atherosclerotic arterial hypotension occurs due to a loss of vascular tone due to atherosclerotic changes.
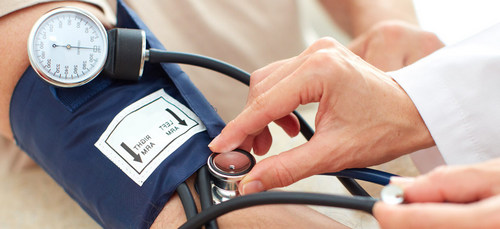
Due to the multifactorial nature of the development of this condition, hypotension is the subject of a study of cardiology, neurology, endocrinology, and other clinical disciplines.
Hypotension – persistent or regular lowering of blood pressure below 100/60 mm. Hg Art. Hypotension occurs with dizziness, transient visual disturbances, fatigue, drowsiness, a tendency to fainting, impaired thermoregulation, etc. Diagnosis of arterial hypotension is based on determining the level of blood pressure (including daily monitoring of blood pressure), examination of the cardiovascular state, endocrine and nervous systems (ECG, EchoCG, EEG, biochemical analysis of blood, etc.). Non-pharmacological (psychotherapy, massage, hydrotherapy, FTL, acupuncture, aromatherapy) and medication (herbal adaptogens, cerebroprotective agents, nootropic drugs, tranquilizers) methods are used in the treatment of hypotension.
Classification of arterial hypotension
Due to the fact that arterial hypotension can occur in healthy individuals, accompany the course of various diseases or be an independent nosological form, a single classification of hypotonic states is used. It secrete physiological, pathological (primary) and symptomatic (secondary) arterial hypotension.
The variants of physiological hypotension include arterial hypotension as an individual norm (having a hereditary constitutional nature), adaptive compensatory hypotension (among residents of highlands, tropics and subtropics) and hypotension of increased fitness (found among athletes).
Pathological primary arterial hypotension, as an independent disease, includes cases of idiopathic orthostatic hypotension and neurocirculatory hypotension with an unstable, reversible course or persistent manifestations (hypotonic disease).
In the series of symptomatic (secondary) arterial hypotension, acute (with collapse, shock) and chronic forms caused by organic pathology of the cardiovascular, nervous, endocrine systems, hematological diseases, intoxications, etc. are considered.
Causes of hypotension
Hypotension should be considered as a multifactorial state, reflecting a decrease in blood pressure in the arterial system under various physiological and pathological conditions.
The cause of primary arterial hypotension in 80% of cases is neurocirculatory dystonia. According to modern theories, primary hypotension is a special form of neurosis of the vasomotor centers of the brain, in the development of which the leading role is given to stresses and prolonged psycho-traumatic situations. The immediate causes can be psychological trauma, chronic fatigue and lack of sleep, and depression.
Secondary hypotension is a symptom of other existing diseases: anemia, stomach ulcers, dumping syndrome, hypothyroidism, cardiomyopathy, myocarditis, arrhythmias, diabetic neuropathy, osteochondrosis of the cervical spine, tumors, infectious diseases, heart failure, etc.
Acute hypotension can be the result of massive single-stage blood loss, dehydration, trauma, poisoning, anaphylactic shock, a sharp disruption of the heart, in which the hypotensive reflexes are triggered. In these cases, arterial hypotension develops in a short time (from several minutes to hours) and entails pronounced disturbances in the blood supply to the internal organs.
Chronic hypotension tends to last for a long time; at the same time, the organism is adapted to reduced pressure, as a result of which there are no pronounced symptoms of circulatory disorders.
Hypotension may also develop on the background of a lack of vitamins B, C, E; dieting, drug overdose, for example, in the treatment of hypertension. Physiological hypotension can be observed in healthy people with a hereditary predisposition to low blood pressure, in trained athletes, in terms of adaptation to an abrupt change in weather or climatic conditions.
Pathogenesis of arterial hypotension
Despite the abundance of possible causes, the mechanism of the development of arterial hypotension may be associated with four main factors: a decrease in the minute and stroke output of the heart; abbreviation BCC; decrease in resistance of peripheral vessels; a decrease in venous blood flow to the heart.
Reducing the stroke and cardiac output is found with severe myocardial dysfunction during myocardial, infarction, severe arrhythmias overdose ß-blockers, etc. D. Reduced tone and peripheral resistance vessels (mainly arterioles and precapillaries) causes the development of hypotension during collapse toxic or an infectious nature, anaphylactic shock.
Hypotension as a result of a decrease in BCC occurs when external (gastrointestinal) or internal bleeding (with ovarian apoplexy, rupture of the spleen, rupture of an aortic aneurysm, etc.). Rapid evacuation of exudate with massive ascites or pleurisy can lead to arterial hypotension due to a decrease in venous blood return to the heart, since a significant part of the BCC is retained in the smallest vessels.
In various forms of arterial hypotension, violations of the vascular regulation by higher vegetative centers, reduction in the mechanism of arterial pressure regulation of the renin-angiotensin-aldosterone system, disorder of vascular receptor sensitivity to catecholamines, disorders of the afferent or efferent part of the baroreflex arc can be detected.
Symptoms of arterial hypotension
Physiological hypotension in most cases does not cause a person special discomfort. The acute form of arterial hypotension occurs with a pronounced oxygen starvation of brain tissue, in connection with which symptoms such as dizziness, short-term visual impairment, unsteadiness of gait, pallor of skin, fainting develop.
In chronic secondary hypotension, the symptoms of the underlying disease come to the fore. In addition, patients have weakness, apathy, drowsiness, fatigue, headaches, emotional lability, memory impairment, impaired thermoregulation, sweating of the feet and palms, tachycardia. A long course of arterial hypotension causes menstrual disorders in women and potency in men.
When orthostatic hypotension due to a change in the position of the body from horizontal to vertical, pre-unconscious states develop. In case of arterial hypotension, vegetative crises can occur, as a rule, of vaginal-insular nature. Such paroxysms occur with adynamia, hypothermia, excessive sweating, bradycardia, a fall in blood pressure and fainting, abdominal pain, nausea, vomiting, difficulty breathing due to spasm of the larynx.
Diagnosis of arterial hypotension
In the process of diagnosis, it is important not only to establish the presence of arterial hypotension, but also to find out the reasons why it is caused. A correct measurement of blood pressure requires a threefold blood pressure measurement at intervals of 3–5 minutes. Daily monitoring of blood pressure allows you to determine fluctuations in the magnitude and daily rhythm of blood pressure.
To exclude or confirm secondary arterial hypotension, a comprehensive examination of the state of the cardiovascular, endocrine and nervous systems is necessary. For this purpose, biochemical blood parameters (electrolytes, glucose, cholesterol and lipid fractions) are examined, an ECG is performed (at rest and with stress tests), an orthostatic test, echocardiography, electroencephalography, etc.
To determine the need for more in-depth examination, patients with hypotension should be consulted by a cardiologist, a neurologist, an optometrist, and an endocrinologist.
Prevention of arterial hypotension
The general principles of prevention of primary arterial hypotension are reduced to the observance of the daily regimen, maintaining a healthy and active lifestyle, playing sports (swimming, walking, gymnastics), good nutrition, elimination of stress.
Useful procedures that strengthen blood vessels (douche, hardening, massage).
Prevention of secondary arterial hypotension is the prevention of endocrine, neurological, cardiovascular diseases. Patients with arterial hypotension are recommended to continuously monitor blood pressure levels, regular monitoring by a cardiologist.



Non-pharmacological (psychotherapy, massage, hydrotherapy, FTL, acupuncture, aromatherapy) and medication (herbal adaptogens, cerebroprotective agents, nootropic drugs, tranquilizers) methods are used in the treatment of hypotension