Still’s disease is a severe Multisystem pathology, the causes and development of which remain unclear. In this disease affected joints are lymphoreticular, cardiovascular and respiratory system of man.
First still disease was first described in the late 19th century, and for many years was regarded as one of the types of juvenile rheumatoid arthritis.
To the 70-th years of the last century has accumulated a lot of information about the possibilities of development of this pathology in adults, although the majority of patients really are children and adolescents up to 16 years.
Treatment is in the competence of specialists-rheumatologists. For therapy used, primarily, NSAIDs, and drugs glucocorticoid hormones, and the funds reserve the cytostatics. Differential diagnosis is carried out using the method of elimination.
Reasons
The exact cause of the disease to the present time is not established. The disease is still characterized by an abrupt onset, suggesting an infectious etiology. However, common to all cases of infectious agent to date not been identified.
Pathogenic microorganisms that were detected in the different patients:

According to some specialists, there is a family (genetically determined) predisposition to the disease. According to genetic theory, the possible link of the disease still violations in the complex of tissue compatibility. Some researchers tend to classify this pathology to autoimmune.
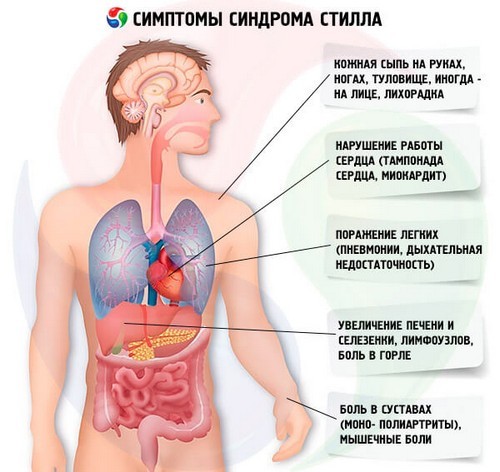
The symptoms still
Leading symptoms still:
- articular syndrome;
- transient skin rashes;
- the febrile reaction (the characteristic “high” fever);
- cardio-pulmonary pathology;
- lose lymphoreticular system (lymphadenopathy and hepatosplenomegaly).
In a laboratory study of the patient’s blood revealed significant leukocytosis with increased levels of neutrophils and increase of erythrocyte sedimentation rate.
Please note that manifestations of the disease are still nonspecific, so patients are often mistakenly diagnosed with “sepsis” and prescribe long courses of antibiotics.
Joint damage
Articular syndrome manifested by arthralgia and myalgia at the peak temperature (joint and muscle pain).

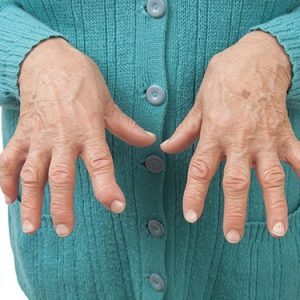
At the initial stage of development of the disease still may be isolated inflammatory involvement of only one joint is arthritis. Further, the process involved and other moving joints, i.e., arthritis develops. It is highly characteristic lesions of the distal interphalangeal joints of the hands. The symptom allows to make a differential diagnosis with SLE, rheumatic fever and rheumatoid arthritis in which the joints in young patients does not suffer.
Fever
The temperature rises to high numbers – 39°C and more, but it is not constantly kept as for most infectious pathologies. Fairly typical of a one-time increase during the day, usually in the evening. In some cases during the day recorded 2 temperature peak. Between them, the temperature returns to normal physiological values; in parallel, to improve your health.
Important: approximately 1 of 5 patients with hyperthermia does not disappear, i.e. fever kept permanently.
Cutaneous manifestations
Transient skin rashes appear at the peak of the fever, and disappear spontaneously with the improvement of the General condition. Most fixed papules (small tight knots) and macula (stain pink). The preferential localization of the rash – proximal parts of arms and legs and torso; in some patients, the skin elements are defined on the face. Approximately 30% of cases they develop in the compression or skin injuries (observed the so-called koebner’s phenomenon). In some cases, patients may complain of itching, but most unpleasant sensations are absent. The rash often remains undetected; in order to reliably confirm its presence in the diagnostics specialist has to resort to provoking heat.
Atypical skin manifestations:
Symptoms of lymphoreticular system
With the disease still suffer lymphoreticular bodies. Almost 70% of patients diagnosed lymphadenopathy; in 50% of cases increased cervical lymph nodes. They retain mobility, as determined by palpation moderately dense consistency.
Important: the cohesion of lymph nodes to surrounding tissues requires further studies to rule out cancer.
In rare cases (atypical course) probably necrotic lymph nodes.
Many of the patients revealed hepatosplenomegaly – significant increase in liver and spleen.
The defeat of the other organs
With the involvement in the pathological process of the respiratory system and heart most often develop inflammation of the serous membranes of organs, pleura and pericardium. Often pleurisy and pericarditis develop in parallel. Every fifth patient is diagnosed with aseptic pneumonitis, which is characterized by symptoms of bilateral pneumonia. Hyperthermia, cough and shortness of breath does not disappear on the background of antibiotic use.

May develop inflammation of the heart muscle; it is also possible cardiac tamponade.
Important: 2/3 of patients complain of a constant burning sensation in the throat. This symptom appears at the beginning of the disease. If the disease is still possible severe vision loss – complicated cataract, ribbon-shaped degeneration of the cornea, or iridocyclitis.
Laboratory parameters
Diagnosing “the disease is still” presents certain difficulties; it in most cases requires prolonged observation of the patient and exclude other pathologies with similar clinical manifestations. Great importance has the study of laboratory data.
Changes in blood tests:
- significant leukocytosis;
- increased ESR (>50 mm/hour).
- the presence of “acute phase proteins” (ferritin, C-reactive);
- increased activity of liver enzymes.
Please note: the result of a bacterial blood culture – negative, which allows to exclude sepsis. Antinuclear and rheumatoid factor are not detected, despite the symptoms that characterized a number of systemic inflammatory diseases.
Data of additional methods of diagnostics
During the x-ray in patients suffering from stilla, revealed the presence of effusion in the joint cavities. Sometimes there is a change in the structure of bone tissue – osteoporosis. If the pathology becomes chronic, the x-ray of the hands visible pattern characteristic of ankylosis.

During puncture of the joint are the synovial fluid with signs of inflammatory reaction; the bacteria in it are not detected.
Differential diagnosis of
To exclude a malignant tumor of the lymph nodes, they are puncture with fence and subsequent cytological and histological study of tissue samples.
If there is a cardio-pulmonary symptoms require additional consultation of specialists in the field of cardiology and pneumology, as well as ultrasound scan of the chest and study of the electrocardiogram.
Pathology, with which differential diagnostics is carried out:
The treatment of the disease still
Medical tactic depends on the clinical course of the disease. In the acute phase pharmacotherapy is carried out with the use of nonsteroidal anti-inflammatory drugs. They have a positive effect in every fourth case. The duration of a course of treatment varies from 1 to 3 months.

In the presence of pathological changes of the heart and respiratory system shows the glucocorticoid is Dexamethasone or Prednisone.
If the disease still takes a chronic course, to reduce the dose of hormones is appointed by the cytostatic agent Methotrexate, which is a structural analogue of folic acid. Backup cytotoxic means that is assigned in severe cases, Cyclophosphamide is.
If the pathology is not amenable to treatment according to the standard scheme can be applied Infliximab an immunosuppressant and a potent immunomodulator Etanercept.
Forecast: recovery from the disease still
Possible outcomes of the disease still can be spontaneous recovery. It occurs in about 30% of patients within 6-9 months. from the appearance of the first symptoms. Often the disease becomes chronic or recurrent form.
In recurrent form, as a rule, there is a single aggravation; less frequently recorded replay attacks.
The hardest flows in the chronic form; it is characterized by symptomatic arthritis with considerable limitation of range of motion in the affected joints.
If pathology develops in adults, a five year prognosis of survival is 90-95%, which is comparable with those in systemic lupus erythematosus. The causes of death may be blood clotting, respiratory distress syndrome, amyloidosis, or secondary bacterial infection (including tuberculosis).


Great ? I should certainly pronounce, impressed with your website.
I had no trouble navigating through all tabs as well as related info ended up being
truly simple to do to access. I recently found what
I hoped for before you know it at all. Quite unusual.
Is likely to appreciate it for those who add forums or something,
web site theme . a tones way for your client to communicate.
Great ? I should certainly pronounce, impressed with your website.
I had no trouble navigating through all tabs as well as related info ended
up being truly simple to do to access. I recently found
what I hoped for before you know it at all. Quite unusual.
Is likely to appreciate it for those who add forums or something, web site theme .