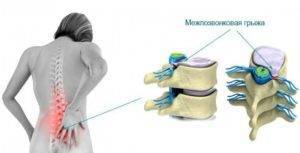
Degenerative changes affecting the intervertebral discs, can hit not only all of this anatomical formation (the fibrous ring and nucleus pulposus), but confined to the external division ring of the disc.
In cases where the patient develops a localized lesion of the outer part of the annulus and tissue of the anterior longitudinal ligament of the spine while maintaining normal structure the rest of the disc located between the vertebral bodies in the lumbar and sacral Department, the physician after performing a comprehensive examination can make a diagnosis of spondylosis of the lumbosacral spine.
Despite the smaller area of lesions per disk, the total surface degenerative changes are more conceived than with the development of diffuse osteochondrosis, hernia and protrusion of disc disease outcome, the occurrence of which is likely in the absence of treatment, makes the development of fusion of the vertebral bodies in one single unit.
Such outcomes can result in significant disability of the patient or the onset of disability therefore, is the importance of timely diagnosis and earlier start of a necessary set of remedial measures.
Why develop spondylosis?
Spondylosis of the lumbosacral spine is a disease that develops in the initial phase as a compensatory reaction in response to excessive load on the vertebral bodies in the place of the greatest congestion occurs a compensatory overgrowth of bone tissue, contributing to reduction of adverse impacts. At the same time develops a spasm of the muscular fibres surrounding the affected area of the spine that can only to a small extent to limit his mobility.
With continued exposure to compensatory-adaptive reaction becomes pathological – gradually increasing the area of contact. Bone growth is gradually developing into the so-called “skirt” – growths-osteophytes, are able to reach huge sizes, and at this stage of development of the disease in the degenerative-dystrophic process can be involved and the anterior longitudinal ligament of the spine. Growths of bone can injure the nerve roots extending from the lumbosacral segment of the spinal cord (lumbar and sciatic nerve) and to raise the shell and the substance of the spinal cord.
At the same time in the tissue of the intervertebral disc there are processes of dehydration – disk structures gradually lose water, which inevitably becomes the reason of further decrease in disc height, and these processes only increase the severity of symptoms in a patient. It is on this principle in spondylosis of the lumbosacral spine developed an intervertebral hernia. At this stage of the disease is spread almost disc between two adjacent vertebral bodies, and the surface area of the disc (cartilage) protrudes from the surface of the vertebral body. Spondylosis deformans develops when running, untreated promptly osteochondrosis of the lumbosacral spine.
Causes of spondylosis may include:
- traumatic injuries (both direct and indirect) of the ligaments and muscles of the spine in the lumbar and sacral Department;
- the static load on the spine – long stay of the body in a physiologically disadvantageous position;
- dynamic loads – short-term physical stress of the muscles surrounding the spine, on the background of pronounced inactivity;
- constitutional and hereditary predisposition;
- age-related changes in the tissues of the spinal column;
- infectious diseases or tumors.
What are the symptoms of this disease?
The most common symptom that can be detected in patients with spondylosis of the lumbosacral spine becomes pain – it can occur while in motion, or intensify during the day, when a sudden change in body position. Some patients may experience some exacerbation of pain when the weather changes (increased meteosensitivity). In the initial stages of the pathological process back pain may be intermittent, possibly periodic spontaneous strengthening and easing discomfort in the affected area of the spine.
In some cases, the first manifestation of the disease may be the development of radicular syndrome and the appearance of signs of damage to the fibres of the lumbar and sacral nerves, and the symptoms of plexitis (inflammation) of the lumbar-sacral plexus. Patients get about “intermittent” claudication (leg pain), which does not disappear in a state of physical rest – it will differ from “limp” resulting from the development of obliterating endarteritis of lower extremities vessels.
With the progression of the changes may appear to limit the range of motion in the vertebrae of the lumbar spine – the degree of restriction will depend on the severity of the spondylosis. Palpation and effleurage on the spinous processes of the vertebrae occurs it is painful, the area distribution which corresponds to the location of the vertebrae and discs involved in the process.
The patient may complain of pain that radiates into the buttocks and lower limbs, weakness in the legs, which may decrease when moving up the ladder or lean forward, because in these processes is a physiological increase in the area of the intervertebral disc.
It is worth remembering that in osteochondrosis, in contrast to spondylosis of the lumbosacral spine, almost never have pain with pressure on the spinous processes of the affected vertebrae.
With the defeat of the lumbosacral spine spondylosis is most often localized in L3-L5, in contrast to the degenerative disc disease affecting the L5-S1 vertebrae.
How does the test work?
To confirm the diagnosis, you will:
- a comprehensive neurological examination of the patient;
- radiographic studies of the spine – images must be executed in standard and lateral projections. This method of research is used to assess the condition of the vertebrae, the detection of osteophytes, abnormal mobility of the individual elements of the spine with extreme degrees of flexion and extension, displacement detection;
- computer and magnetic resonance tomography is used to determine the height of the intervertebral disc, the width of the spinal canal and its condition.
A comprehensive treatment of spondylosis
Treatment should be comprehensive and take into account all the features of the patient – it should be directed to:As with detection of any other disease of the spine, the doctor when the diagnosis of this disease should appoint his patient’s comprehensive treatment plan, which will aim to prevent the progression of degenerative changes in cartilage and bone tissue.

It is important to remember that self-medication in this disease may worsen the condition of the tissues of the spine and limit the ability of the patient.
- Improving the condition of the cartilage of the intervertebral disc.
- The restoration of blood supply and innervation of tissues of the spine and intervertebral disc.
- Relief of significant pain syndrome.
- Reduce friction and pressure of the vertebrae.
- Strengthening of muscular-ligamentous apparatus of the spine.
For the treatment can be used medicines, mainly in the acute stage (for relief of pain syndrome), such methods of treatment, such as:
- Acupuncture (relief)
- Electrophoresis (but only the device “Yonason”)
- Hivamat (is the pain for 2 sessions)
- Applique Ozokerite