Acanthameba – protozoal damage to the eyes, skin and CNS caused by free-living amoebas. The disease occurs in the form acanthamoebae conjunctivitis and keratitis, dermatitis or granulomatous encephalitis. Complications of acanthamebiasis can serve as perforation of the cornea, the formation of abscesses of internal organs.
The diagnosis of acanthamebiasis is established by the detection of amoebae and their cysts in the lacrimal fluid, scrapings from cornea, skin biopsies, cerebrospinal fluid.
Local and systemic treatment of acanthamebiasis conducted by the aminoglycoside antibiotics group (in the form of eye drops, ointments, injections).
Acanthameba
Acanthameba – protozoos caused by pathogenic amoebae of the genus Acanthamoeba. In most cases, Acanthamoeba takes the form acanthamoebae acanthameba keratitis and skin lesions. Sporadic cases acanthamoebae dermatitis are more often registered in countries with subtropical and tropical climates. Acanthameba keratitis usually occurs in people who use contact vision correction.
Acanthamoebae rarely diagnosed granulomatous encephalitis. In the world has registered about 400 cases of acanthamebiasis occurring with lesions of the Central nervous system; survival in this form is only 2-3%. Thus, Acanthamoeba is an actual interdisciplinary problem to be solved by specialists in ophthalmology, dermatology and neurology.
Causes of acanthamebiasis
Among free-living pathogenic amoebae of the genus Acanthamoeba danger to humans 6 species: A. hatchetti (cause eye damage), A. palestinensis, and A. astronyxis (cause CNS), A. polyphaga, A. Culbertsoni, A. castellanii (cause various lesions including skin). In the process of the life cycle of an amoeba of the genus Acanthamoeba are the vegetative stage (trophozoite) and the stage of the cysts.
Acanthameba – aerobic organisms living in soil, freshwater stagnant water natural and artificial water bodies, especially contaminated waste waters. In addition, unicellular protozoa live safely in the tap water, sewage, water from the heating pipes. The increase in the population of Acanthamoeba contributes to water temperatures above 28°C and the presence of various organic substances. In the case of reducing the ambient temperature or the drying up of the reservoir of Acanthamoeba incestious. Able cysts parasites tolerate fluctuations in temperature and pH, the effects of antiseptics and disinfectants.
When injected into the human body the causative agents of acanthamebiasis once again pass into a vegetative state and become capable of parasitism. The source of infection are contaminated acanthamoebae soil and water. Human infection is contact-household, food and waterways. Acanthameba eye usually occurs in patients who do not observe hygienic rules of wearing and caring for soft contact lenses: do not remove them during bathing and showering, neglecting the measures of disinfection, not processing the hands before putting on lenses, etc. in healthy people Acanthamoeba often found in nasopharyngeal mucus and faeces, however, the development of acanthamebiasis the Central nervous system affected mainly persons with immunodeficiency (especially HIV infection), diabetes, malignant neoplasms, alimentary insufficiency.
Symptoms of acanthamebiasis
Acanthameba most often takes the form acanthameba keratitis. The initial symptoms of eye infections include redness of the eye, cutting the eye pain, photophobia, lacrimation, blurred vision, foreign body sensation in the eye. In the later period becomes noticeable discoid or annular corneal opacity. The alternation of exacerbations and remissions when acanthamebiasis eyes often leads to uveitis, scleritis, iridocyclitis, hypopyon. Without adequate treatment acanthamebiasis progresses rapidly, causing perforation of the cornea.
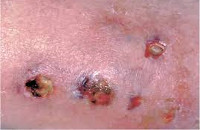
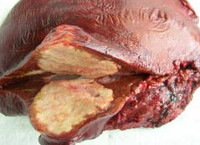
Acanthomas of the skin may occur primary (self) or secondary, due to the initial damage to the Central nervous system. Primary acanthamoebae skin lesions occurs by ingestion of water contaminated with cysts of amoeba, on the open sores of the skin. While on the face, chest, back, limbs are formed of single or multiple nodules, papules, or spots of greyish-black, reaching a diameter of 0.5-3 cm. In the future, these elements transformirovalsya in ulcers of the skin, covered with a scab. In the long acanthameba the formation of abscesses of the muscles, lymph nodes, liver, lungs and other internal organs. Secondary acanthomas of the skin caused by the dissemination of acanthameba of the primary tumor.
CNS when acanthamebiasis causes the development acanthamoebae granulomatous encephalitis. This rare pathology usually occurs when there is hematogenous drift of acanthameba to the brain from primary tumors. Amoebic lesion may affect the substance of the brain, vascular or arachnoid, basal ganglia. Under normal resistance of the organism develops granulomatous inflammation; reduced necrotic process. The incubation period for Acanthamoeba the brain damage lasts from several weeks to a month or more. The initial period of acanthamebiasis is characterized by intermittent low-grade fever, drowsiness, headaches, convulsions, impaired convergence. The progression of acanthamebiasis the Central nervous system leads to coma and death.
Diagnosis and treatment of acanthamebiasis
Depending on the shape of acanthamebiasis its diagnosis and treatment is carried out by specialists, ophthalmologists, dermatologists, neurologists. Diagnosis acanthamoebae damage to eyes, skin, brain, confirmed by the detection of vegetative and cistych forms of Acanthamoeba in the material. When Acanthamoeba keratitis is tears, swabs and scrapings of the cornea; dermatitis Acanthamoeba – detachable infiltrates, biopsies of the skin; granulomatous encephalitis – spinal fluid. In addition to microscopical preparations, to verify the diagnosis of acanthamebiasis applied culture method serological test biological sample. If you suspect Acanthamoeba should be deleted from the patient keratitis, encephalitis, and dermatitis of different etiology.
Treatment acanthameba keratitis requires refusal of wearing contact lenses. Local therapy includes hourly instillation in the conjunctival cavity of antibacterial drugs (gentamicin, neomycin, polymyxin b, etc.), corticosteroids, use of antifungal agents (amphotericin b, ketoconazole). In combination with eye drops uses ointment application over the eyelid these funds. In progressive changes of the cornea can be shown holding keratoplasty.
When acanthamebiasis skin systemic antibiotic treatment with drugs of the aminoglycoside, local application of ointments with neomycin, polymyxin b, etc. the Most difficult task is therapy acanthamoebae encephalitis. In this clinical form of acanthamebiasis shown intravenous amphotericin b, administration of a combination of trimethoprim and sulfamethoxazole, aminoglycosides. Treatment of CNS acanthamebiasis is effective only in isolated cases.
Forecast and prevention of acanthamebiasis
When Acanthamoeba lesions of the skin and eyes the prognosis for life is favorable, however acanthameba of the brain in the majority of cases ends in death. Prevention acanthameba keratitis is in compliance with the rules of use and care for contact lenses, storage only in sterile solutions, the handling of containers for lenses, periodic instillation into the eye of microbicides (sulfatsil sodium, etc.), you need to remove contact lenses while swimming, visiting the baths and saunas, washing in the shower. To prevent Acanthamoeba skin and Central nervous system enables the personal hygiene, limiting contact with contaminated reservoirs, which are habitats of acanthameba.



You could definitely see your expertise in the work you write. The world hopes for even more passionate writers like you who aren’t afraid to say how they believe. Always go after your heart.
One other issue is when you are in a problem where you don’t have a co-signer then you may really want to try to make use of all of your financing options. You can find many awards and other grants that will supply you with money to support with college expenses. Thx for the post.
I was suggested this web site by my cousin. I’m not sure whether this post is written by him as no one else know such detailed about my difficulty. You’re wonderful! Thanks!
After reading your blog post, I browsed your website a bit and noticed you aren’t ranking nearly as well in Google as you could be. I possess a handful of blogs myself, and I think you should take a look at “seowebsitetrafficnettools”, just google it. You’ll find it’s a very lovely wordpress SEO tools that can bring you a lot more visitors and improve your ranking. Keep up the quality posts
After reading your blog post, I browsed your website a bit and noticed you aren’t ranking nearly as well in Google as you could be. I possess a handful of blogs myself, and I think you should take a look at “seowebsitetrafficnettools”, just google it. You’ll find it’s a very lovely SEO tool that can bring you a lot more visitors and improve your ranking. They have more than 30+ tools only 20$. Very cheap right? Keep up the quality posts
Great post, you have pointed out some superb points, I likewise conceive this s a very fantastic website.
when did this happen?
After reading your blog post, I browsed your website a bit and noticed you aren’t ranking nearly as well in Google as you could be. I possess a handful of blogs myself, and I think you should take a look at “seowebsitetrafficnettools”, just google it. You’ll find it’s a very lovely SEO tool that can bring you a lot more visitors and improve your ranking. They have more than 30+ tools only 20$. Very cheap right? Keep up the quality posts
Thank you for your own hard work on this website. My mom delights in making time for investigations and it is simple to grasp why. A number of us learn all relating to the compelling way you provide valuable steps by means of your web blog and therefore attract participation from people about this content then my child is really understanding so much. Take pleasure in the remaining portion of the year. Your performing a really good job.
I抦 not sure where you are getting your info, but good topic. I needs to spend some time learning more or understanding more. Thanks for magnificent information I was looking for this information for my mission.
Great wordpress blog here.. It’s hard to find quality writing like yours these days. I really appreciate people like you! take care
I’m really enjoying the design and layout of your blog. It’s a very easy on the eyes which makes it much more enjoyable for me to come here and visit more often. Did you hire out a designer to create your theme? Exceptional work!
Good post! We are linking to this great content on our website. Keep up the great writing.