Disc herniation is one of the most common and severe complications of degenerative disc disease. After the formation of hernial protrusion is accompanied by severe pain syndrome and neurological symptoms – numbness and tingling in the extremities, impaired urination and defecation, disorder of erection.
The age of patients suffering from illness, 30-60 years, and hence the recovery and restoration of health must be a priority in the treatment of degenerative disc disease.
Methods of treatment of hernias of a backbone there are conservative and operative. Conservative methods include medication, physiotherapy, massage, medical gymnastics. The course of treatment is rather long, but effective.
Surgical treatment
In some situations, you cannot avoid interference of the surgeon.
Operative treatment is indicated in the following situations:
- hernia is large and sequestered, so there is a complete loss and separation kernel;
- the spinal cord compression and neurological symptoms such as numbness and disorders of pelvic organs;
- severe pain, which is poorly removed painkillers;
- the absence of effect of conservative therapy for two months.
Today all types of operations for hernia of the spine are divided into traditional and non-traumatic. The choice of method of surgical intervention depends on the age and condition of the patient, symptoms of the disease, its impact on daily life and human performance.
The classic ways
Traditional types of operations in case of intervertebral hernia include:
- Discectomy – removal of a disc of the spine along with a herniated spine which compresses the spinal cord. Replacement of the removed cartilage is installed the titanium prosthesis, which ensures the stability of the vertebrae. In the future, the adjacent vertebrae are fused together. This type of intervention has the disadvantages of: the wound is large enough, but recovery after surgery is long.
- Laminectomy – removal of part of the affected vertebra it arches. This eliminates the compression of the spinal cord or its nerve roots. A significant disadvantage of this type of intervention is the instability of vertebrae, injury to the joints between the vertebrae, a high risk of recurrence of a hernia.
These operations are performed under anesthesia. Discharge from hospital after traditional interventions occurs in one to two weeks, then for two months are prohibited a seat and work, and physical activity contraindicated for up to three months. The first months after surgery, patients are recommended to wear the corset.
Minimally invasive surgery
Microsurgical resection of a disk between the vertebrae using an operating microscope. This technique is optimal in hernia surgery of the spine. Because the likelihood of injury of nerve trunks during surgery, and spinal instability with microdiscectomy minimal, the statement may be carried out at 2-5 day, and two weeks later the patient returns to light work.
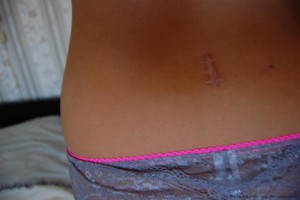
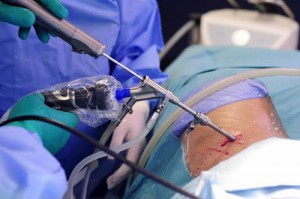
Endoscopic microdiscectomy is performed with special tools under visual control of a miniature camera of the endoscope. Access to the hernia through a small puncture, and therefore, the operation is practically harmless. The risk of complications is reduced, and the recovery period after surgery is minimal. The clinic, the patient leaves on the day after the intervention and almost immediately he is ready to start working. And physical exertion and heavy lifting is possible after 2-4 weeks.
Destruction of nerves of the intervertebral joints (facet nerves) – microsurgical manipulation. Nerves are inactivated by radiofrequency waves. The procedure is performed under local anesthesia, takes about half an hour. After surgery pain syndrome docked immediately, and the patient can return home.
Laser surgery
Laser destruction of the intervertebral disc that is not running effectively at an early stage of the disease. The laser beam produces evaporation (vaporization) of the disc, the pressure therein is reduced, the hernia decreases in size. The method is particularly suitable for young patients.
Disk recovery laser irradiation of the intervertebral structures in a special mode, whereby the cells of the cartilage begin to grow and divide. The disk status is improved, the pain stopped. The procedure is effective after surgery, to prevent recurrence of hernial protrusion.




Everything is very open and very clear explanation of issues. was truly information. Your website is very useful. Thanks for sharing.
Spot on with this write-up, I truly believe that this amazing site needs a lot more attention. I’ll probably be back again to see more, thanks for the advice!