Acute pancreatitis is a painful and very dangerous disease. Symptoms of it are almost impossible to endure “on the feet”: this is a strong persistent pain under the spoon and under the left rib, which often gives back (there is the so-called girdle pain).
A person with acute pancreatitis often even occupies a special position on the bed – lies on his left side so as not to aggravate the pain with the movements of the ribs during breathing.
Most people with acute pancreatitis experience severe nausea and vomiting, any meal increases the pain: after all, the pancreas begins to secrete enzymes when it is eaten, and this increases blood flow, which means pain. Many people have a fever.
Not every abdominal pain is pancreatitis. And it pleases.
Pancreatitis is an inflammation of the pancreas. This organ secretes enzymes in the duodenum (just behind the stomach) that help food digest: for example, amylase (for breaking down carbohydrates) and lipase (for breaking down fats). With severe inflammation of the pancreas – acute pancreatitis – its cells are destroyed and enzymes enter the bloodstream. Therefore, for any severe abdominal pain, doctors determine the amylase content in the blood.
Diagnosis of acute pancreatitis is not so much for gastroenterologists as for surgeons, since the intensity of pain can be the same as with appendicitis and other “surgical” pathologies.
How does acute pancreatitis occur?
About 70% of all cases of acute pancreatitis occur either due to alcohol poisoning, or due to gallstone disease. Excessive alcohol consumption (even without a history of alcoholism) causes inflammation of the pancreas. For the same reason, people who systematically abuse booze have every chance not only to be in a hospital with severe acute pancreatitis, but also to experience pain attacks for many years.

Gallbladder stone can also cause pancreatitis: the duct that carries bile from the bladder to the duodenum 12 merges with the duct of the pancreas. This situation – biliary pancreatitis – requires emergency intervention, for example, to dissect a large duodenal papilla: this is the place where the ducts enter the intestine.
Acute pancreatitis can also cause the toxic effects of certain drugs, gland injury during surgery, or high blood fats. It is extremely rare and, as a rule, in the presence of other similar diseases, the pancreas becomes inflamed due to the excessive action of the immune system on it.
Whatever the cause of the onset of the disease, acute pancreatitis is always accompanied by abdominal pain. It is not worthwhile to suggest this diagnosis if a malady appears from a medicine or some product.
With acute pancreatitis sorted out. A chronic?
If the toxic effect on the pancreas does not stop (for example, the person continues to abuse the drink) or the organ was very badly damaged during the first (acute) episode of pancreatitis, the pain resumes again and again.
With exacerbations of chronic pancreatitis, blood tests may remain normal. But over time, external signs may appear that doctors find when examining the pancreas using ultrasound (ultrasound), x-ray (CT, or computed tomography) or magnetic resonance imaging (MRI). This is a narrowing of the pancreatic ducts, the appearance in it of seals – calcifications, as well as the appearance of cysts – bubbles with fluid in place of dead tissue. Screening for suspected chronic pancreatitis is carried out with another important goal – not to miss cancer of the pancreas, which may initially be accompanied by the same symptoms.

With constantly recurring inflammation of the pancreas, its function is disrupted over time – the release of enzymes that digest food. As a result, a person is worried about constant bloating, diarrhea, and the stool becomes oily (for example, it is poorly washed off the toilet). This condition – exocrine insufficiency – is most conveniently detected by determining the content of pancreatic elastase (pancreatic enzyme) in the stool.
How to treat chronic pancreatitis
In general, the meaning of the treatment of chronic pancreatitis is to eliminate the pain. To do this, use anti-inflammatory drugs, such as paracetamol. Often, people with chronic pancreatitis are prescribed enzymes. Alas, this does not always relieve pain. It was previously assumed that adding enzymes to food would reduce the load on the pancreas – it would not have to secrete its own enzymes. In fact, everything is not so simple: the secretory (excretory) activity of the gland depends entirely on other substances – hormones, for example, secretin. Their products are more affected by the fat content of the food and the regularity of its intake than the content of enzymes-drugs in the gut.
Nevertheless, enzymes for chronic pancreatitis must be prescribed (often for life), if there are signs of poor secretion of their own enzymes (bloating, loose stools). Enzymes always drink directly with food: “between the spoons.” For the same reason, it is illiterate to prescribe the intake of enzymes “so many times a day.” It is more correct to warn a person with a disease that the drug should be carried with you and taken with any food intake.
A diet for chronic pancreatitis eases the course of the disease, although it is difficult to determine the exact list of possible foods the first time. It is definitely impossible to drink unless alcohol, but they traditionally recommend eating less fatty foods and snacking more often, preferring slow carbohydrates – fruits and vegetables. Steaming exclusively is not the most proven way to alleviate the course of pancreatitis, it is much more important not to abuse very spicy foods. Roughly speaking, there will most likely be no harm from the chicken cutlet, even if cooked without copious seasoning.
The main thing in the treatment of chronic pancreatitis is to remove the cause of the disease. If a person suffers from alcoholism or smokes, refer him to a narcologist (smoking in itself does not cause pancreatitis, but it often exacerbates). If pancreatitis happened due to stones in the gallbladder, remove the bladder. If the body has a fat metabolism disorder, consult a cardiologist and choose a treatment with drugs that lower the level of lipoproteins and triglycerides, and choose a diet.
Most of my friends have been diagnosed with pancreatitis, but they don’t drink alcohol and have never been to the hospital with severe pain. What’s wrong?
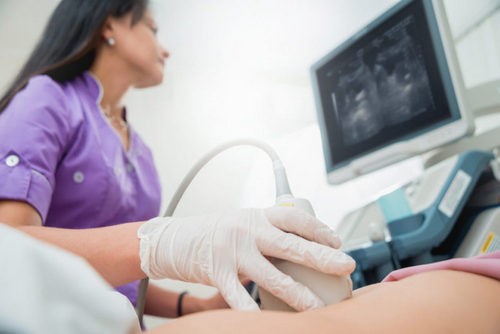
Most likely, like many other Russians, the diagnosis of pancreatitis in this situation was made solely by ultrasound. A competent specialist in ultrasound diagnostics will not establish a diagnosis for a therapist, gastroenterologist or surgeon. He will only describe the changes and invite his colleague to interpret the changes in the pancreas himself. Often, the so-called diffuse changes in the pancreas become an occasion to diagnose pancreatitis in humans without any symptoms at all. It is not right.
Reliably judge pancreatitis with ultrasound, strictly speaking, you can only detect obvious complications of the disease – narrowing and expansion of the duct, calcifications, cysts.
Yes, and the ultrasound method, like any diagnostic method, the possibilities are not unlimited. With real pancreatitis, preference is given to magnetic resonance or endoscopic cholangiopancreatography. With these methods, a very accurate image of the pancreatic ducts is obtained.
Diffuse changes in the pancreas most often turn out to be quite harmless accumulation of adipose tissue in the gland. In the absence of typical symptoms of chronic pancreatitis – exhausting pain after eating in a person who has already suffered acute pancreatitis once, such an ultrasound picture should only become an occasion to check cholesterol and, perhaps, actively fight overweight.
In addition, very often for chronic pancreatitis take the most common diseases in gastroenterology – functional disorders, such as irritable bowel syndrome. This is a non-dangerous, but very unpleasant disease, in which the intestine becomes too sensitive to stretching with gas and food, responding with spasm (colic).
Very often, such functional pain (that is, pain not associated with inflammation or swelling) occurs in people who are under constant stress. Therefore, the treatment of functional pain is not only the use of antispasmodic drugs and other gastroenterological drugs, but also work with the psycho-emotional state: cognitive-behavioral psychotherapy, increased physical activity, and even yoga.



