In newborns, jaundice appears 2-3 days after birth. Doctors believe that yellowish tint is normal physiological nature. This symptom disappears after adjustment of the liver to the cleansing function.
Postnatal jaundice occurs in 98% of infants. During intrauterine development of the child is not breathing (lack of oxygen). To use only the amount of oxygen the red blood cells of the fetus should work on fetal hemoglobin.
Its composition is most similar to the chemical composition of oxygen. When a child is born, his fetal hemoglobin is replaced by the standard. Then there is the cleansing of the body from the old hemoglobin. Red blood cells are diagnosed excess of bilirubin.
The clinical picture
Pediatricians are the following reasons for emergence of zheltushki in infants:
- heredity, weak body, the adjustment of the child for adult life;
- the strong decay of red blood cells (hemolytic jaundice), bleeding during childbirth;
- chronic and infectious disease, a low concentration of substances involved in the metabolism of bilirubin.
Substance into the blood, contributes to the staining of the skin in yellow. This substance is non-toxic and well-excreted in the urine. Jaundice in children term disappears 7 days after birth, otherwise within 10-14 days.

Pediatricians are the following types of jaundice in preterm infants and normal children:
- Conjugational – develops on the background of asphyxia, endocrine pathologies.
- Drug (heredity).
- Hemolytic – immunology antigens of red blood cells the mother and the baby.
- Nuclear – for this pathology there is increased concentration of bilirubin. For the diagnosis of abnormalities is carried out a full examination of the baby.
- Mechanical – develops on the background of violations of the outflow of bile and biliary tract malformation, and tumors. This pathological form is manifested a few days after birth. Thus, symptoms such as green skin, enlarged spleen. The disease is diagnosed by ultrasound, biopsy and cholangiography.
The distinctive characteristics of pathological jaundice physiological forms:
- vomiting yellow;
- yellow skin;
- the appearance of yellow spots and yellowing of the whites of the eyes.
The above symptoms of jaundice occur in month babies and observed for 3 weeks. When is the neonatal form of the disease, it is recommended to find out from the doctor. The symptoms of neonatal jaundice, in contrast to the pathological, are alone for several days. When the diagnosis treatment is not required.
Form of pathology
Prolonged neonatal jaundice is characterized by the main symptoms that are observed in 2-3 weeks. Dangerous complication of this form is neurotoxic shock. Physiological jaundice of the newborn is a frequent phenomenon, which is observed in approximately 75% of infants. In 25% of cases, the bilirubin has not time to collect in such numbers to dye the skin.
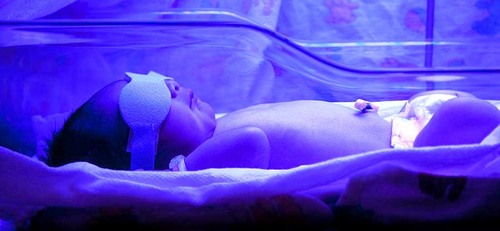
If the baby shows the first signs of jaundice, then the parents have to monitor its condition (round the clock). At high concentrations of bilirubin excreted chemical which later turns to poison. Developing nuclear jaundice. It affects the brain and Central nervous system. This pathology is diagnosed in 5% of full-term children and in 10-20% of preterm babies.
Treatment of obstructive jaundice is the surgery, medication and physiotherapy. Your doctor will tell you when needs to go through pathology. Therapy physiological jaundice is associated with getting colostrum. Breast milk is rich in vitamins and trace elements, promoting faster recovery of the baby. A premature baby is placed in the hospital. To reduce the concentration of bilirubin using a UV lamp. This substance is excreted from the body in a natural way. If necessary, the baby is put on a drip with glucose or phenobarbital (to speed up development and running of bilirubin).
Hemolytic jaundice in infants develops (from the first minute of birth) because of the incompatibility of rhesus monkey mother and fetus. Treatment is assigned based on the General condition of the baby. Causes of jaundice in the newborn may be related to the fact that the fetus has a blood group of father. This pathology is diagnosed in every 2-3 children.
Medical termination of pregnancy provokes rapid formation of antibodies, which affect the subsequent pregnancy.
Complications and prevention of the disease
Hemolytic disease is dangerous because the child’s condition worsens by the day:
- poor appetite;
- long sleep;
- lethargy;
- anemia;
- seizures during sleep (due to lesions of the nervous system).
Children who survive hemolytic alfalfa butterfly, often lag behind in development. The manifestation of this pathology in the edematous form dangerous premature birth, miscarriage or stillborn baby. In mild course of the disease, anemia, pale skin.

Hemolytic jaundice in newborns treated in a hospital. To eliminate antibodies formed during the first hours of baby’s life need to transfuse blood. If necessary, the procedure is performed 2-3 times.
A child is prescribed drugs that enhance the functioning of the liver. A baby is fed (within 2 weeks) expressed milk someone else’s mother, as in the body home mom observed elevated levels of antibodies. A child needs special care.
Children’s jaundice, in contrast to adult disease (viral hepatitis), is not transmitted. The baby often prescribe activated charcoal. But you cannot take this drug without consulting your pediatrician. This is due to the fact that the Activated carbon is greatly dehydrates the body, quickly destroying the walls of internal organs.
To prevent the child’s jaundice is recommended during pregnancy to live a healthy lifestyle. An expectant mother with a negative rhesus factor should always be under the supervision of a physician (monthly testing for antibodies).




Way cool, some valid points! I appreciate you making this article available, the rest of the site is also high quality. Have a fun.